Determinants Of Surgery Analysis
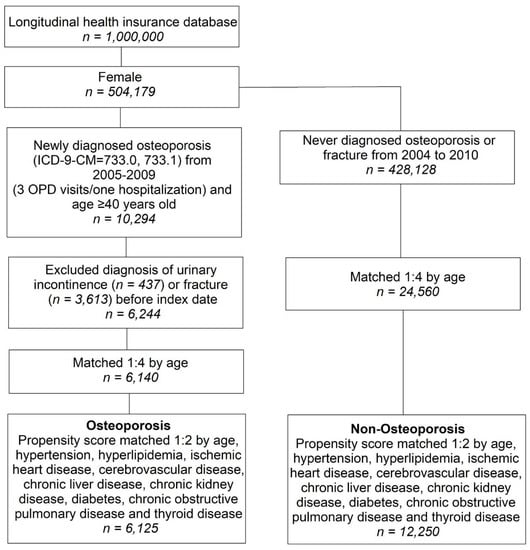
The cohort for identifying determinants of surgery after referral comprised women aged 18 years who had an index UI diagnosis and a referral to a urinary incontinence specialist in secondary care between 1 April 2004 and 31 March 2014. The cohort of women for surgery after referral was derived from the CPRD linked to HES APC data set and was therefore restricted to women registered in primary care practices that had linked CPRDHES data. Women were followed up from the date of referral until the date of surgery, transfer out of practice, death or to 1 April 2014.
Outcome measures
Determinants of referrals analysis
For the determinants of referrals analysis, the outcome measure was referral to a UI specialist within 30 days of diagnosis.
Determinants of surgery analysis
For the determinants of surgery analysis, the primary outcome measure was risk of any UI surgery.
Potential determinants of referral and surgery
Statistical analyses
Determinants of referrals analysis
For the determinants of referrals analysis we used multivariate logistic regression, with cluster standard error estimands to account for clustering within general practices, to identify factors associated with referral within 30 days.
Determinants of surgery analysis
What Is Urinary Incontinence And How Is It Related To Prostate Cancer Surgery
Urinary incontinence is the loss of the ability to control urination . Urinary incontinence sometimes occurs in men whove had surgery for prostate cancer.
If youve had prostate cancer surgery, you might experience stress incontinence, which means you might leak urine when you cough, sneeze or lift something that is heavy. This happens because of stress or pressure on the bladder. There is also a type of incontinence that is called urge incontinence. When this happens, you are hit with a sudden need to urinate right away and have leakage before you can make it to the bathroom.
Read Also: Urinary Incontinence In Child Treatment
Periurethral Injections Of Bulking Agents
You May Like: Urinary Tract Infection Does It Go Away On Its Own
Other Experimental And Investigational Interventions For Urinary Incontinence
Quality Payment Program Measures
When code N39.3 is part of the patient’s diagnoses the following Quality Measures apply and affect reimbursement. The objective of Medicare’s Quality Measures is to improve patient care by making it more: effective, safe, efficient, patient-centered and equitable.
| Quality Measure | ||
|---|---|---|
| Percentage of female patients aged 65 years and older with a diagnosis of urinary incontinence with a documented plan of care for urinary incontinence at least once within 12 months. | Person and Caregiver-Centered Experience and Outcomes | Process |
You May Like: How Does A Urinary Tract Infection
N399 Disorder Of Urinary System Unspecified
NEC Not elsewhere classifiableThis abbreviation in the Tabular List represents other specified. When a specific code is not available for a condition, the Tabular List includes an NEC entry under a code to identify the code as the other specified code.
NOS Not otherwise specifiedThis abbreviation is the equivalent of unspecified.
This note further define, or give examples of, the content of the code or category.
List of terms is included under some codes. These terms are the conditions for which that code is to be used.The terms may be synonyms of the code title, or, in the case of other specified codes, the terms are a list of the various conditions assigned to that code.The inclusion terms are not necessarily exhaustive. Additional terms found only in the may also be assigned to a code.
Certain conditions have both an underlying etiology and multiple body system manifestations due to the underlying etiology.For such conditions, the ICD-10-CM has a coding convention that requires the underlying condition be sequenced first, if applicable, followed by the manifestation.Wherever such a combination exists, there is a use additional code note at the etiology code, and a code first note at the manifestation code.These instructional notes indicate the proper sequencing order of the codes, etiology followed by manifestation.
Urinary Incontinence: Treatment Involved
Your treatment plan will depend on your incontinence. Underlying medical issues will demand surgery or medication. Rarely, do medical professionals fail to cure incontinence but they will suggest some methods to manage your situation effectively. Treatment plans for urinary incontinence include:
- Bladder training: You will be recommended pelvic floor exercises to control your bladder better.
- Behavior therapy: Behavioural therapy involves managing your fluid intake, using the bathroom at scheduled times, adjusting your diet, etc. .
- Condition management: If there is an underlying condition of your incontinence such as UTI or constipation, you will be treated for the condition which will cure your incontinence as well.
- Medication: Sometimes, you can cure your incontinence with medicines but it depends on the causes. Antimuscarinics are a set of drugs that treat an overactive bladder.
- Catheter placement: If the incontinence is persistently affecting your quality of life, you will be suggested an external or internal catheter to manage the overflow.
- Weight loss: losing weight also helps in treating urinary incontinence because it relieves the pressure on your bladder.
- Absorbent undergarments: Using absorbent undergarments or pads also help in managing small leaks.
- Reducing bathroom barriers: If you are having physical trouble navigating toward the bathroom, it could lead to urinary incontinence. So maintain a well-lit and obstacle-free path to help you get there ASAP.
You May Like: Back Pain Causing Urinary Problems
Enuresis Not Due To A Substance Or Known Physiological Condition
- 20162017201820192020202120222023Billable/Specific Code
- 20162017201820192020202120222023Billable/Specific Code
Code Also
- 20162017201820192020202120222023Non-Billable/Non-Specific Code
- any associated overactive bladder
- urinary incontinence associated with cognitive impairment
- urinary incontinence NOS
- 20162017201820192020202120222023Billable/Specific Code
Applicable To
- stress incontinence and other specified urinary incontinence
- urinary incontinence NOS
- Applicable To annotations, or
Screening For Urinary Incontinence In Women
Despite the lack of studies determining the benefits and harms of UI screening, the Women’s Preventive Services Initiative recommended that doctors screen women of all ages, including adolescents, for UI yearly by using a questionnaire. The WPSI recommended referring women with UI for further evaluation if it affects their activities and QOL. These recommendations were based on indirect evidence that UI is common, treatment may be effective, and the harms of screening are unlikely to be serious. The recommendations might change if studies directly evaluating the benefits and harms of screening for UI become available. There are no data to support that the correct frequency of screening is yearly .
Don’t Miss: Sling Procedure For Male Urinary Incontinence
Transcutaneous Electrical Nerve Stimulation In The Treatment Of Overactive Bladder
In a randomized, double-blind, placebo-controlled study, Borch and associates evaluated the immediate effect on natural fill urodynamic parameters and bladder function during TENS in children with OAB and daytime UI . A total of 24 children with severe OAB and DUI underwent 48-hour natural fill urodynamics. After 24hours of baseline investigation, the children were randomized to either active continuous TENS or placebo TENS over the sacral S2-S3 outflow. The urodynamic recordings were analyzed manually for 3 different bladder contraction patterns resulting in a void. The number of bladder contractions not leading to a void was also calculated. Maximum voided volume and average voided volume were identified for both the baseline and the intervention day. It was found that TENS had no immediate objective effect on bladder capacity. The difference in MVV/EBC in the active TENS group=0.03±0.23 versus placebo TENS group=-0.01±0.10 . Furthermore, there was no significant difference in the proportion of different bladder contraction types between the 2 groups TENS did not significantly influence the number of bladder contractions not leading to a void. Results were presented as mean±SD. The authors concluded that there was no immediate objective effect of TENS on bladder activity assessed by natural fill urodynamics in children with OAB and DUI.
What Kinds Of Surgeries Treat Urinary Incontinence After Your Prostate Is Removed
There are two types of surgery for urinary incontinence: the urethral sling and the artificial urinary sphincter. Usually, the incontinence needs to last for about one year after the prostatectomy to be sure there is not going to be further improvement before your healthcare provider suggests this type of therapy.
You May Like: Laser Treatment For Urinary Incontinence
When To Seek Medical Help
All instances of urinary incontinence are a sign to seek medical help as it could be a symptom of an underlying disease. Even if the underlying cause is a non-serious issue, incontinence can turn out to be a major disruption of your daily life. An accurate diagnosis and treatment are required to treat it. Some cases of incontinence are a sign of a medical emergency so keep an eye out for them:
- Loss of bowel control
- Tingling or weakness in any part of your body
- Trouble walking or speaking
Coding Notes For R3981info For Medical Coders On How To Properly Use This Icd
- Inclusion Terms:
Inclusion Terms
Inclusion Terms are a list of concepts for which a specific code is used. The list of Inclusion Terms is useful for determining the correct code in some cases, but the list is not necessarily exhaustive.
- Urinary incontinence due to cognitive impairment, or severe physical disability or immobility
- Code Type-1 Excludes:
Type-1 Excludes
Type-1 Excludes mean the conditions excluded are mutually exclusive and should never be coded together. Excludes 1 means do not code here.
You May Like: Are Probiotics Good For Urinary Tract
Magnetically Controlled Endourethral Artificial Urinary Sphincter
Mazzocchi and colleagues stated that UI is a widespread dysfunction that affects more than 300 million people worldwide. At present, no technological solutions are able to restore continence in a minimally invasive and effective way. These researchers described the design, fabrication, and testing of a novel artificial endourethral urinary sphincter that attempts to fully restore continence. The device can be inserted/retracted in a minimally invasive fashion without hospital admission, does not alter the body scheme and can be applied to both women and men. The device core is a uni-directional polymeric valve and a magnetically activated system, which is able to modulate its opening pressure. Bench tests and ex-vivo tests on a human cadaver demonstrated that the device was able to fully restore continence and allowed urination when desired. The authors concluded that the proposed system showed a high potential as a technological solution that may restore a normal daily life in patients affected by UI. These preliminary findings need to be validated by well-designed studies.
Test Stimulation Of The Interstim
The InterStim product labeling states that, in clinical studies, subjects underwent anywhere from 1 to 6 test stimulation procedures before implantation of InterStim.
The Medtronic InterStim test stimulation lead kit manual stated that Of the 260 patients who qualified for implantation, 169 had a successful result during their first test stimulation procedure. Of the remaining 91 patients, 56 obtained a successful result during a second test stimulation, and 35 obtained a successful result during three or more test stimulations. Reasons for repeat test stimulation procedures included inadequate responses to test stimulation or technical problems . The safety and effectiveness of this therapy has not been established for pediatric use , patients with neurological disease origins, such as multiple sclerosis or diabetes, and bilateral stimulation.
Read Also: Homeopathic Cure For Urinary Tract Infection
What Is An Artificial Urinary Sphincter And How Does It Help With Urinary Incontinence
An artificial urinary sphincter can help men who have moderate to severe urinary incontinence due to poorly functioning muscle or sphincter valve after prostate cancer surgery.
The AUS has three parts:
- An inflatable cuff that is placed around the upper urethra. The cuff closes off the urethra to prevent leakage of urine.
- A pump that is inserted into the scrotum. Its completely on the inside and not visible, and the pump controls the opening and closing of the cuff.
- A small pressure-regulating balloon that is placed in the abdomen, under the muscles. The balloon maintains fluid under pressure within the urethral cuff to pressurize the system and hold urine back.
If you have this surgery, youll press on the pump when you feel the need to pee. This opens the cuff to allow urine to pass. When youre done peeing, the cuff automatically closes again on its own.
The AUS procedure provides a very good and satisfactory result in 90% of cases. Risks are uncommon and include:
- Failure of the device .
Axonics Neuromodulation System For The Treatment Of Urinary Incontinence
Wang et al noted that over-active bladder and UUI affect millions of women and men and results in billions of dollars in health-care expenses. First- and 2nd-line therapy includes behavioral modifications and/or pharmacotherapies however, many patients’ symptoms remain or worsen on these treatments. There has been concern regarding the detrimental side effects of the most widely prescribed medications for these bladder symptom management. As a result, there has been increased interest in continuous sacral neuromodulation, an FDA-approved therapy for refractory UUI. These investigators reviewed current research on the effectiveness and patient/provider satisfaction and safety profile of the Axonics System. Furthermore, they addressed the current state SNM and potential future direction and applicability. The authors concluded that the Axonics system is a safe and effective device for the treatment of OAB and UUI. In additional, it affords patient’s the convenience of a rechargeable, compact, MRI safe system. It should be noted that the rechargeable system, while allowing for approximately 15 years of battery and lead life, may have its challenges in terms of charge burden. Furthermore, this system is easily adapted for experienced implanters of sacral neuromodulating devices.
Don’t Miss: Royal Canin Urinary S O Moderate
The 4 Types Of Urinary Incontinence And How They Are Diagnosed
If youve ever leaked urine or had trouble getting to the bathroom quickly enough, youre not alone. Almost half of all women leak urine at some point in their lives a condition known as urinary incontinence.
Urinary incontinence can be frustrating and embarrassing. Fortunately, treatment can make a difference. At Virtuosa GYN in San Antonio, Texas, Dr. Susan Crockett offers patients with urinary incontinence a full range of treatment options, from lifestyle changes and exercise to medication and surgery.
To give you a better understanding of your condition, Dr. Crockett offers the following information about the main types of urinary incontinence, along with details about what causes them and how they are diagnosed and treated.
Other Urinary Incontinence Interventions
Pelvic Muscle Trainers
Note: Aetna does not cover the Athena pelvic muscle trainer, Gyneflex, Kegelmaster, Leva Pelvic Floor Trainer, or similar devices for the treatment of UI because these devices are considered exercise machines, and they do not meet Aetna’s definition of covered durable medical equipment . Most Aetna plans exclude coverage of exercise devices. Please check benefit plan descriptions for details. In addition, such exercise devices do not meet Aetna’s definition of covered DME because they are not primarily medical in nature and/or are normally of use to persons who do not have an illness or injury.
You May Like: Prescription Medicine For Urinary Tract Infection
What Is A Urethral Sling Procedure And How Does It Help With Urinary Incontinence
In the urethral sling procedure, a synthetic mesh tape is placed around part of the urethra, moving the urethra into a new position. This is a minimally invasive procedure, which means that the surgeon only has to make a small incision in the perineum .
Your provider may recommend a urethral sling procedure if you have mild to moderate urinary incontinence after a radical prostatectomy that hasnt improved using other more conservative measures. Its highly successful in helping men overcome incontinence, or reduce episodes of leaking urine.
Before the surgery, the provider may do some tests, including the following:
- A urodynamic study, to test how well the bladder is working.
- A 24-hour pad test .
- A cystoscopy, a test in which the doctor looks inside the bladder with an instrument called a cystoscope.
You dont have to donate any of your own blood before surgery.
You May Like: What Causes Frequent Urinary Tract Infections