Causes Of Urinary Tract Infections
Urinary tract infections are usually caused by bacteria from poo entering the urinary tract.
The bacteria enter through the tube that carries pee out of the body .
Women have a shorter urethra than men. This means bacteria are more likely to reach the bladder or kidneys and cause an infection.
Things that increase the risk of bacteria getting into the bladder include:
- having sex
-
do not use scented soap
-
do not hold your pee in if you feel the urge to go
-
do not rush when going for a pee try to fully empty your bladder
-
do not wear tight, synthetic underwear, such as nylon
-
do not drink lots of alcoholic drinks, as they may irritate your bladder
-
do not have lots of sugary food or drinks, as they may encourage bacteria to grow
-
do not use condoms or a diaphragm or cap with spermicidal lube on them try non-spermicidal lube or a different type of contraception
Possible Symptoms And Complications Of A Kidney Infection
A kidney infection can be acute or chronic, depending on the duration of the problem. An acute kidney infection is commonly seen to develop in just a few hours or maximally 24 hours. Patients usually have very high body temperature , experience some shivering, feel sick, vomit and suffer from pain in the lower back. Some people suffering from pyelonephritis may also experience different problems with urination: stinging, burning and the urge to urinate frequently and urgently. There might also be some blood in the urine or a change of color and smell .
Pregnant women, diabetes patients and elderly people, as well as people with a weakened immune system, urinary catheter or persistent kidney infection are considered to be high risk groups for the development of complications after kidney infections caused by E.coli. These patients may suffer from swelling of the kidneys, kidney abscesses or even sepsis .
Biofilm Production By Upec
Biofilm production by E. coli is an important VF which may also protect bacteria from antibiotic action and so contribute to resistance . Recent studies have shown that biofilm production in E. coli , mediated by co-expression of curli and cellulose, supports long-term survival of UPEC in the urinary tract by surrounding the organism with an inert, hydrophobic extracellular matrix . Most studies of biofilm formation in UTI have addressed its role in recurrences.
Curli belong to a class of fibers known as amyloids and are involved in adhesion to surfaces, cell aggregation and, finally, biofilm development. Curli fibers are encoded in the curling subunit gene gene cluster, made up of two differently transcribed operons. One operon codes for csgB, csgA , and the other one for csgD, csgE , and csgG . Expression of both curli operons is important for curli fiber assembly. Curli fibers are also essential for internalization of bacteria during an infection .
Also Check: One Piece Male External Urinary Collection Device
Vaccines Targeting Bacterial Toxins And Proteases
The UPEC pore-forming toxin HlyA has also received attention as a potential vaccine target and was evaluated in a mouse model of pyelonephritis to assess protection against renal damage,. Vaccination with HlyA reduced the incidence of renal scaring compared with controls however, it did not protect against UPEC colonization of the kidneys. In addition, in a mouse model of UTI, vaccination with the P. mirabilis haemolysin, HpmA, did not provide protection against bacterial colonization. However, vaccination with Pta, an alkaline protease with toxic effects towards epithelial cells, displayed promising results in a mouse model of UTI, protecting against upper UTI, although bacterial burdens in the bladder remained unaffected. Thus, although haemolysins and proteases might provide effective vaccine targets for preventing upper UTIs, additional studies are needed to determine the effectiveness of these enzymes as targets for vaccines.
Are There Distinct Upec Pathotypes
Individual genes or even clusters of genes encoding a single complete virulence factor are not by themselves sufficient to allow bacteria to cause disease. Rather, complementary sets of virulence factors work together to direct bacteria through a particular interaction with the host that can result in disease. Strains of a given bacterial species that have a particular set of virulence factors in common that direct them through a particular pathogenesis process are called a pathotype. As mentioned earlier, E. coli causing enteric/diarrhoeal disease can be grouped into at least six different pathotypes. What is the evidence that E. coli causing UTIs may also be made up of distinct pathotypes?
After removing pathotype 1 strains from the analysis, cnf1 and hly are still strongly associated with each other , and with sfa as well . Further, hly also appears to be associated with papGAD/IA2, an association that does not exist when all isolates are compared . Therefore, we defined all strains that were cnf1+hly+sfa+, after the removal of pathotype 1 strains, as pathotype 2 strains. The strains containing cnf1 are almost always grouped as either pathotype 1 or pathotype 2. When the pairwise association analysis was performed on the remaining strains after removal of both pathotype 1 and 2 strains, hly was positively associated with papGAD/IA2 at a level that reaches statistical significance in each of the collections .
Also Check: Best Way To Get Rid Of Urinary Tract Infection
Treatment For Uncomplicated Utis
UTIs can often be successfully treated with antibiotics prescribed over the phone. In such cases, a health professional provides the people with 3 to 5-day antibiotic regimens without requiring an office urine test. This course is recommended only for women who have typical symptoms of cystitis, who are at low risk for recurrent infection, and who do not have symptoms suggesting other problems. It is always best to have a urine culture done before starting antibiotics when possible.
Antibiotic Regimen
Oral antibiotic treatment cures nearly all uncomplicated UTIs, although the rate of recurrence remains high. To prescribe the best treatment, the doctor should be made aware of any drug allergies of the person.
The following antibiotics are commonly used for uncomplicated UTIs:
After an appropriate course of antibiotic treatment, most people are free of infection. If the symptoms do not clear up within the first few days of therapy, doctors may suggest an alternate course of antibiotics. This may depend on the result of the urine culture. A urine culture may be ordered in order to identify the specific organism causing the condition if not done prior to starting antibiotics.
It should be noted that resistance to many of the commonly used antibiotics is growing and this is why it is now recommended to culture the urine before starting antibiotics. This helps reduce the overuse of these medications.
Treatment for Relapsing Infection
Mechanisms Of Action And Resistance To Anti
Because tetrahydrofolate is required to make both purines and pyrimidines, its synthesis is important for understanding the mechanism of cotrimoxazole, which is a combination of trimethoprim and sulfamethoxazole. Trimethoprim is a structural analog of dihydrofolic acid that competitively inhibits the synthesis of tetrahydrofolic acid. Sulfamethoxazole, which has a sulfonyl group instead of a carbonyl group, is an analog of para-aminobenzoic acid that competitively inhibits the synthesis of dihydrofolic acid. Over two decades after its first use in 1974 , this drug has remained the first-line treatment for uncomplicated UTIs in adults . Because of the widespread resistance to the drug, cotrimoxazole has been gradually replaced by fluoroquinolones since approximately the year 2000 . The mechanism of bacterial resistance to cotrimoxazole is due to drug efflux pumps, the degradation of the antibiotics by enzymes, the alteration of antibiotic binding targets, and the loss of drug entry points, all of which can occur via chromosomal mutations or the acquisition of plasmids .
OXA family -lactamases hydrolyze oxacillin at a faster rate than that observed for benzylpenicillin. OXA-related -lactamases have recently been identified in plasmids from E. coli that exhibit low-level resistance to imipenem and resistance to ertapenem. Plasmid-mediated dissemination of OXA-48-like carbapenemases in E. coli has been observed in many European countries .
You May Like: Causes Of Urinary Incontinence In Elderly Males
Urine Culture With E Coli: Meaning Results And Treatment
Different microbes such as viruses, fungi, and bacteria can cause a urinary tract infection. Bacteria are the most common culprits even though your body has a natural defense system to throw these bacteria out of your body when they enter your urinary tract. But, sometimes, your natural defense fails, giving bacteria the chance to cause an infection in the urethra , bladder , or kidneys . To confirm your symptoms are due to a urinary tract infection, your doctor will ask for a urine test in which they will look for E. coli.
Escherichia Coli And Kidney Infection
The common harmful bacteria Escherichia coli are very frequently found to be the cause of pyelonephritis. These bacteria live in the bowels of healthy people, and through the urethra they could travel into the bladder and the ureters , causing infections of the lower urinary tract , such as cystitis or kidney infections.
Women are more vulnerable to developing a UTI, because of their anatomy which makes the urethra nearer to the anus and also shorter than in men.
Kidney infections may develop in patients without a prior bladder problem, especially due to the blockage of the kidneys and conditions such as enlarged prostate or kidney stones. Additionally, the infection may also come to your kidneys from some other part of the body.
Recommended Reading: Urinary Tract Infection Blood Clots
Also Check: How To Treat Urinary Incontinence After Prostate Surgery
Relationship Between Antibiotic Resistance And Virulence Or Phylogenetic Background In Upec
Previous studies show that in E. coli isolates from patients with urosepsis, resistance to antimicrobial agents such as ampicillin, sulfonamides, tetracycline, chloramphenicol, and streptomycin is negatively associated with virulence and a phylogenetic group B2, but positively associated with host compromise . There is a similar negative association between FQ resistance and VFs and group B2 . This suggests that, resistance may provide a greater fitness advantage to E. coli than traditional VFs or a group B2 background, allowing them to cause infections in compromised hosts with weakened defenses who are frequently exposed to antibiotics.
What Causes A Urinary Tract Infection
Urinary tract infections are caused by microorganisms usually bacteria that enter the urethra and bladder, causing inflammation and infection. Though a UTI most commonly happens in the urethra and bladder, bacteria can also travel up the ureters and infect your kidneys.
More than 90% of bladder infection cases are caused by E. coli, a bacterium normally found in the intestines.
Read Also: Mens Urinary Health Supplements
Recommended Reading: How Can A Guy Get A Urinary Tract Infection
Treating An Uncomplicated Uti Caused By E Coli
Treatment options vary widely for UTIs, however the conventional treatment is antibiotics, in particular fluoroquinolone. Antibiotic resistance is an issue, with multi-drug resistant Enterobacteriaceae, mostly E. coli, being a matter of concern.
E. coli strains are resistant to penicillins and cephalosporins, as well as fluoroquinolones and gentamicin. Non-antibiotic treatments that can be applied at home include herbal medicines, reflexology, and others, but ongoing or severe infection, especially involving the kidneys, requires prompt medical attention.
Awareness Of Asymptomatic Bacteriuria
ABU should be distinguished from symptomatic UTI. ABU occurs in an estimated 1-5% of healthy pre-menopausal females, increasing to 4-19% in otherwise healthy elderly females and men, also occurring in 0.7-27% of patients with diabetes, 2-10% of pregnant women, 15-50% of institutionalized elderly patients, and 23-89% of patients with spinal cord injuries . ABU does not cause systemic influences, such as renal damage . Thus, treatment of ABU is not recommended in patients without risk factors . Furthermore, ABU should not be overtreated without the awareness of the physician . Even in catheterized patients , antibiotics should be considered only when patients with indwelling catheters present symptoms or they have any complications during placement or exchanges of catheters . In contrast, considering ABU in pregnancy, many researches recommended treating the UTIs because not to treat UTIs in pregnant women can increase the possibilities of preterm labor or low birth-weight .
Don’t Miss: Canine Urinary Tract Infection Home Remedies
E Coli Uti Pathogenesis
UTI pathogenesis is a complex process that is influenced by various host biological and behavioral factors, and by properties of the infecting pathogen, including VFs. This presents a challenge in epidemiological studies regarding the role of specific VFs in UTI pathogenesis because of the confounding effect of host factors.
In most noncompromised individuals, the urinary tract is normally sterile, and the entry of exogenous microorganisms is prevented by urine flow, secreted and tissue-associated antibacterial factors, and the bactericidal activities of effector immune cells. In most cases, the host fecal flora is the source of the infecting E. coli strain, and spreads via the perineal, vaginal, and periurethral areas to the lower urinary tract where they may establish colonization . Two hypotheses have been proposed to explain the movement of the organism from the fecal flora to the urinary tract. The prevalence hypothesis holds that the numerically most prevalent E. coli clones in the feces will be involved, whilst the pathogenicity theory holds that E. coli strains with enhanced virulence potential will be selected . These two mechanisms may not be mutually exclusive, but instead may jointly contribute to UTI pathogenesis .
How Did I Get Infected With E Coli
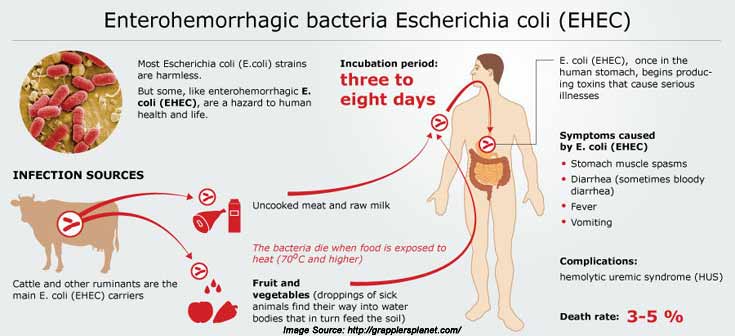
You come into contact and swallow E. coli by eating contaminated food, drinking contaminated water or by touching your mouth with your hands that are contaminated with E. coli bacteria.
Contaminated foods
- Meats: Meats become contaminated with E. coli during the slaughtering process, when E. coli in animal intestines gets onto cuts of meat and especially when meat from more than one animal is ground together. If you eat undercooked meat , you can become infected with E. coli.
- Unpasteurized milk: E. coli on a cows udder and/or the milking equipment can get into the milk. Drinking contaminated raw milk can lead to an E. coli infection because it hasnt been heated to kill the bacteria.
- Unpasteurized apple cider and other unpasteurized juices.
- Soft cheeses made from raw milk.
- Fruits and veggies: Crops growing near animal farms can become contaminated when E. coli-containing animal poop combines with rainwater and the runoff enters produce fields and lands on the produce. If you dont thoroughly wash off the produce, E. coli enters your body when you eat these foods.
Contaminated water
- E. coli in poop from both animals and humans can end up in all types of water sources including ponds, lakes, streams, rivers, wells, swimming pools/kiddie pools and even in local city water supplies that have not been disinfected. If you swallow contaminated water, you could get sick.
Contaminated hands
Don’t Miss: What Antibiotic Do You Take For Urinary Tract Infection
Can You Get A Uti From Having Sex
Sexual intercourse is a prime scenario for bacteria to enter the urethra, especially for women, who tend to experience more UTIs than men do. The physical activity involved in sex can send bacteria into the urethra. In fact, studies show that increasing the frequency of sex increases the likelihood of UTIs. Remember that the urethra connects directly to the bladder, so if the germs continue to travel up the urinary tract, they will reach the bladder first.
Sex is a common way for germs like bacteria to enter the urinary tract, but its not the only way. Lets discuss some other potential UTI causes.
The kidneys are key organs that filter the blood and eliminate waste products, while keeping essential minerals and substances to distribute to the rest of the body. All the waste from the blood leaves the body via urine. Both kidneys or one kidney may get infected with a variety of harmful bacteria, causing pyelonephritis the medical name for a bacterial kidney infection). Very often, E. coli is responsible.
Statistical Analysis Of Communities
The CFU/mL count for all bacteria in each of the 63 independent samples containing one of the sequenced E. coli genomes were examined. The individual contributing 3 isolates to our collection of E. coli genomes was removed from consideration as they are not independent samples. In addition to these data, we included CFU/mL counts for the urobiomes that we have previously characterized from samples of women with UTI symptoms and women without LUTS. In total, this resulted in 109 participants with UTI symptoms and 90 participants with no LUTS. CFU/mL data was recorded at the genus level rather than the species level for our analysis. To analyze prevalence of UTI among participants, a multiple logistic regression model was used. We treated the no LUTS group as our baseline category for the UTI group. For each participant, abundances of 27 different bacteria were measured genera appearing in only one sample were removed from consideration. Abundance of these 27 species of bacteria were treated as covariates in our model. Akaike Information Criterion was used to reduce the full model. All analyses were conducted in R4.
Also Check: Urinary Tract Infection Treatment Without Antibiotics
Check If It’s A Urinary Tract Infection
Symptoms of a urinary tract infection may include:
- pain or a burning sensation when peeing
- needing to pee more often than usual during the night
- pee that looks cloudy, dark or has a strong smell
- needing to pee suddenly or more urgently than usual
- needing to pee more often than usual
- lower tummy pain or pain in your back, just under the ribs
- a high temperature, or feeling hot and shivery
- a very low temperature below 36C
Small Compounds Targeting Urease
Urease, an enzyme which catalyzes the hydrolysis of urea, is crucial in the pathogenesis of several uropathogenic bacteria such as P. mirabilis, Klebsiella sp., Pseudomonas sp. and Staphylococcus sp. . This enzyme leads to the alkalinization of the urine and the production of struvite and carbonate apatite that make up the major component of urinary stones . These conditions lead to the inflammation of the urogenital epithelia thus increasing the risk of catheter-associated biofilm formation that may contribute to pyelonephritis , mainly due to both bacterial and host cysteine protease .
The most studied inhibitors of urease are hydroxamic acids . These molecules have a high inhibitory activity against urease, by bonding to the two nickel ions in the urease active site . Initially, these molecules were used to treat UTIs by preventing urine alkalization . However, because of the growing evidence of side effects such as mutagenic power, they were progressively phased out .
Through similarly interacting with nickel ions in the urease active site, the phenyl phosphoramidates were found to have the highest inhibitory activity . Studies testing these molecules in an in vitro model and in a rat model found promising results. Since then, no in vivo studies or clinical trials have been developed, probably due to the poor hydrolytic stability of these molecules which leads to a very short half-life .
Read Also: Itching In Urinary Area Female Home Remedy