Join Our Community Sign Up To Our Newsletter
Restorative Medicine
Restorative medicine is an evidence based, scientifically sound medical sub-speciality. Its goal is to extend lifespan, prolong youthspan, and healthspan, through early detection, prevention, treatment, and reversal of all age-related dysfunctions, disorders, and disease, in both men and women alike. Restorative medicine has been embraced by thousands of physicians. Menopause Woman does not provide medical advice, diagnosis or treatment. See more information.
Follow Us
Will Probiotics Help Prevent Utis
While it might seem like taking oral probiotics chock-full of Lactobacilli would be the best answer, De Nisco isnt optimistic. Oral probiotics are unlikely to colonize the urinary tract because they must survive and establish themselves within the gastrointestinal tract first, she says. Probiotic suppositories might be a more efficient route to the urinary tract, but more research is needed, she says.
Hormone Therapy Has Health Benefits And Risks
Additional research, including randomized trials, needs to be done before HT is deemed a preventive tool for UTIs in post-menopausal women, De Nisco says. This research would strive to determine a causal relationship between estrogen therapy, Lactobacillus colonization, and the prevention of UTIs rather than simply an association, she says.
Hormone therapy has risks and benefits, and the decision to start it must be made by each woman and her doctor with her unique health history in mind, says Susan Todd Peeler, MD, a gynecologist with Mercy Medical Centers Institute for Gynecologic Care in Annapolis, Maryland. The potential benefit these researchers uncovered might just be another check mark in the plus column, she says.
One less risky delivery system is vaginal estrogen therapy, in which the hormone is used topically. Women with vaginal dryness who are at increased risk of breast cancer, stroke, or blood clots from hormone therapy sometimes use this method, Dr. Peeler notes. Systemic hormone therapy has a significantly different risk benefit profile than hormones used vaginally, she says.
In this study, however, women taking systemic HT via patches or orally had more Lactobacilli in their urine than those using a vaginal cream, so its not clear that method would be sufficient.
RELATED: Some Hormone Therapies Are More Effective Than Others in Preventing Heart Disease
Also Check: Iams Proactive Health Urinary Tract Health
Personal Story: How I Managed My Recurrent Utis During Perimenopause
In my mid-40s I started having UTI symptoms every time I had sex. I felt I was always at the doctor and had 11 courses of antibiotics to treat UTIs in one 12-month period. I cant describe the sheer humiliation of having to go to the loo every 30 minutes it limited enjoyment of life and put me off sex. My doctor really helped me try different ideas and we worked out it was latex and some lubes that triggered it. My husband had a vasectomy so we didnt have to worry so much about contraception and it has made a huge difference! Also, I always pee after sex!
Tessa
Why Incontinence With Menopause

Your bladder sits above your pelvic bones and is supported by your pelvic floor. The pelvic floor is less of a floor and more of a sling of tendons and muscles that support your internal organs. Think of a hammock of muscles that run between the pubic bone in the front, and stretches back to the tailbone at the back.
A womans pelvic floor muscles support her uterus, bladder, and colon. The bladder relaxes and fills with urine throughout the day. If it is working properly, the small opening that opens and closes to release urine will keep the bladder closed until you can use the bathroom. During pregnancy and then menopause, your pelvic floor muscles will be less able to hold the urine in and the sphincter can open unexpectedly.
With age, and as a woman gets closer to menopause, hormone levels drop steadily. Hormones work to keep your bladder and urethra healthy. Lower levels of estrogen and testosterone can cause pelvic floor muscles to become weak. As these hormone levels continue to drop during menopause, UI symptoms can become worse.
Urge Incontinence is a little different than stress incontinence. Urge incontinence causes women to lose control entirely or too quickly. They might feel the urge to go but are not able to reach a bathroom in time. The relationship between your menopause and bladder results in an overactive bladder, which urges you to pee constantly.
Don’t Miss: What Causes Urinary Urgency And Frequency
Depression And Mood Swings
Changes in hormone production affect the moods of women during menopause. Some women report feelings of irritability, depression, and mood swings, and often go from extreme highs to severe lows in a short period of time. Its important to remember that these hormone fluctuations affect your brain and that feeling blue is not unnatural.
Also Check: Mckesson Disposable Urinary Leg Bag
Utis In Menopause All You Need To Know
UTIs are fairly common and affect about half of women at least once in their lives. They occur when bacteria enter the urinary tract and multiply. This can happen when the urinary tract is not completely emptied, which allows bacteria to grow. The incidence of UTIs in menopausal women is significant and it demands some serious attention. In this article, we will discuss what UTI is and how it should be coped with in menopause.
Don’t Miss: Demanos For Urinary Tract Infection
Prescription Antibiotics From Your Healthcare Provider
If you are experiencing the symptoms of a UTI, you should call your physician. Most physicians will treat UTIs with antibiotics that can be called directly into the pharmacy without an in person visit. If you have had multiple UTIs or are not sure if what you are experiencing is a UTI, an in-person visit where you can be evaluated for other causes and can leave a urine sample may be the best option. It is very important that you not start antibiotics if you need to leave a urine sample. Even one or two doses is enough to invalidate your results. Typically you will need to take an antibiotic for 1 to 3 days and you should experience significant improvement of your symptoms within 24 hours.
The Emotional Side Of Urinary Tract Infections
Taking more time for ourselves also means addressing our emotions. In mind-body medicine, one school of thought proposes that bladder pain and infection can represent the trapped expression of anger or frustration in ones life. I shared this theory with one sweet-natured woman who suffered from recurrent UTIs, and her response was, Oh, that is me to a T no wonder! Along with drinking lots of water and getting to the bathroom frequently, it certainly cant hurt to work on a full range of emotional expression instead of bottling things up inside.
Some women may be frightened or embarrassed to discuss urinary tract infections with their doctors. As I mentioned earlier, women in perimenopause and menopause, as well as those who are breastfeeding, may have low estrogen levels, which can leave vaginal tissues vulnerable and more fragile. Yet many avoid asking for help due to fears about hormone replacement therapy or surgery. Fortunately, there are several low-risk natural estrogen options that can be used locally to significantly lower the risk and complications of UTIs .
Read Also: Mckesson Disposable Urinary Leg Bag
Also Check: How Can Urinary Tract Infection Be Treated
Why Are Menopausal Women More Prone To Utis Genitourinary Syndrome Of Menopause
As you go transition into menopause, your bodys production of estrogen begins to decline and your estrogen levels fluctuate and eventually decrease. These hormonal changes affect your urinary tract, vaginal tract, and vulva in ways that can make you prone to developing UTIs. These physical changes and the symptoms associated with them are known as the genitourinary syndrome of menopause .
When Urinary Tract Infections Keep Coming Back
If you are prone to recurrent UTIs, you can head them off before they take hold.
Unless youâre in the fortunate minority of women who have never had a urinary tract infection , you know the symptoms well. You might feel a frequent urgency to urinate yet pass little urine when you go. Your urine might be cloudy, blood-tinged, and strong-smelling. For 25% to 30% of women whoâve had a urinary tract infection, the infection returns within six months.
If you have repeated UTIs, youâve experienced the toll they take on your life. However, you may take some comfort in knowing that they arenât likely to be the result of anything youâve done. âRecurrent UTIs arenât due to poor hygiene or something else that women have brought on themselves. Some women are just prone to UTIs,â says infectious diseases specialist Dr. Kalpana Gupta, a lecturer in medicine at Harvard Medical School.
Read Also: Can A Bladder Infection Cause Dizziness
Don’t Miss: Benefits Of Cranberry Juice For Urinary Tract Infection
You Can Look Out For The Following Symptoms To Confirm A Urinary Tract Infection:
- Burning like sensation while urinating
- Foul odor from the urine
- Very frequent urge to urinate
- Dark-colored urine
- Uneasiness because of the incomplete passage of urine out of the body
To your surprise, the home remedies for urinary tract infections are quite simple to bring in effect. So, lets begin with the best home remedies to use for curing urinary tract infections in males.
Recommended Reading: What Juice Helps Urinary Tract Infections
What Causes Urinary Tract Infection
The vast majority of urinary tract infections are caused by the bacteria Escherichia coli , which is usually found in the digestive system. However, other pathogens may cause a UTI. These include:
- Klebsiella pneumonia
- Enterococcus faecalis
- Staphylococcus saprophyticus
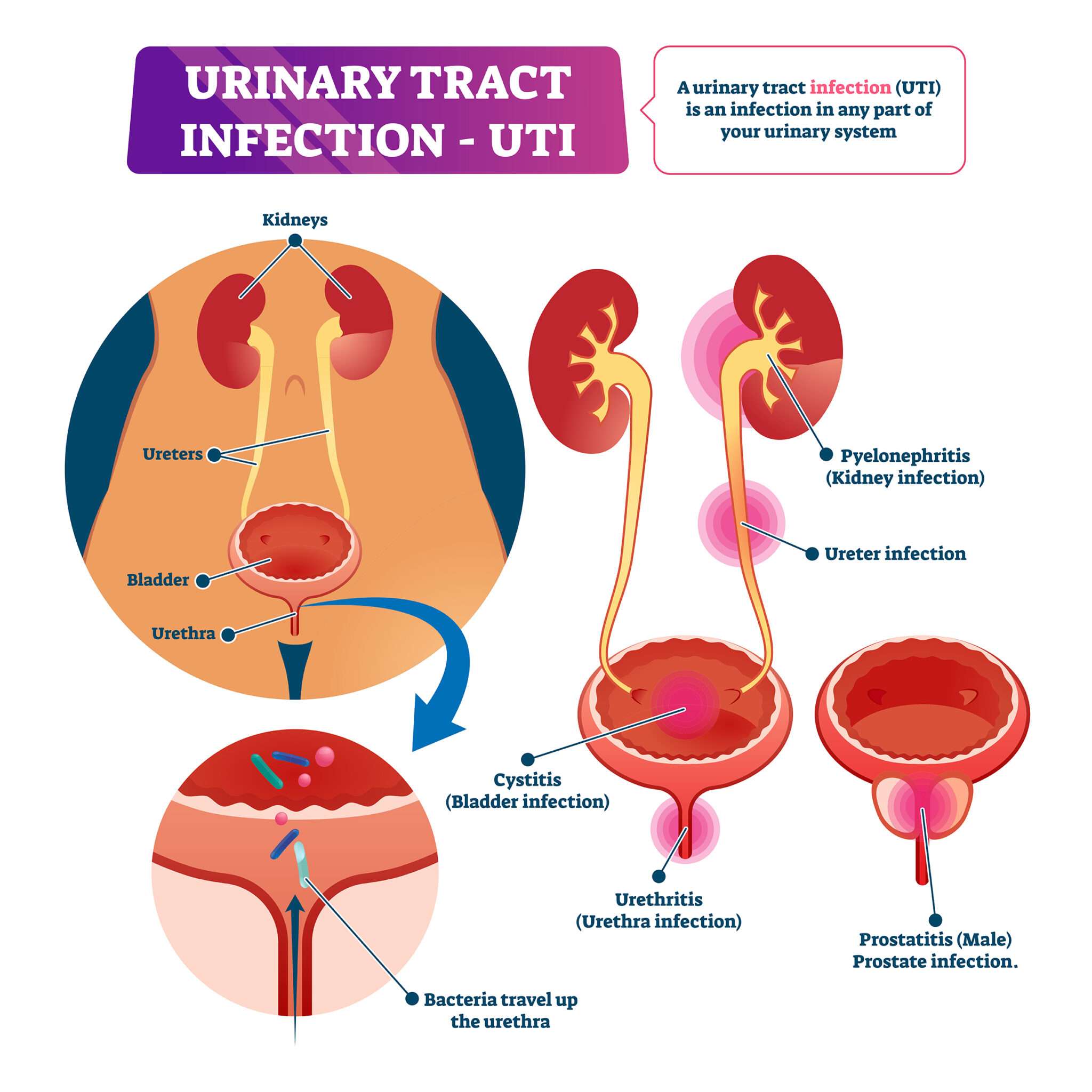
The bacteria may infect any part of the urinary tract bladder, urethra or kidneys. Depending on where the infection occurs, the UTIs are often known as:
- Cystitis infection of the bladder
- Urethritis infection of the urethra
- Pyelonephritis infection of the kidneys
The infection in urethra and bladder is usually not very serious and clears up with treatment. Similarly, ureters very rarely get infected. However, if a UTI reaches the kidneys, it may lead to kidney infections and a person may have to go to the hospital for treatment.
Recommended Reading: What Is The Treatment For Low Grade Bladder Cancer
Don’t Miss: Does Cranberry Juice Cure Urinary Tract Infections
Study Sheds New Light On Urinary Tract Infections In Postmenopausal Women
- Date:
- UT Southwestern Medical Center
- Summary:
- A new study suggests why urinary tract infections have such a high recurrence rate in postmenopausal women: several species of bacteria can invade the bladder walls.
A UT Southwestern study suggests why urinary tract infections have such a high recurrence rate in postmenopausal women: several species of bacteria can invade the bladder walls.
UTI treatment is the most common reason for antibiotic prescriptions in older adults. Because of the prevalence of UTIs, the societal impact is high and treatment costs billions of dollars annually.
âRecurrent UTI reduces quality of life, places a significant burden on the health care system, and contributes to antimicrobial resistance,â said Dr. Kim Orth, Professor of Molecular Biology and Biochemistry at UTSW and senior author of the study, published in the Journal of Molecular Biology.
The investigation demonstrates that several species of bacteria can work their way inside the human bladderâs surface area, called the urothelium, in RUTI patients. Bacterial diversity, antibiotic resistance, and the adaptive immune response all play important roles in this disease, the study suggests.
Since the advent of antibiotics in the 1950s, patients and physicians have relied on antibiotics for UTI treatment.
The latest findings build on decades of clinical UTI discoveries by Dr. Zimmern, who suggested the collaboration to Dr. Orth, along with other UT System colleagues.
Story Source:
Treatments For Menopausal Urinary Symptoms
Systemic HT may reduce the urinary symptoms of urgency, frequency, nocturia and painful urination, but there is continuing debate about the effectiveness of systemic HT in treating urogenital atrophy.
Local estrogen, applied externally, is helpful in relieving the symptoms of urinary urgency, frequency and stress incontinence, and can also help prevent urogenital atrophy and the recurrence of urinary tract infections.
The most common treatment for vaginal atrophy symptoms is low-dose vaginal estrogen replacement, utilizing creams, tablets or vaginal rings.
However, some women are not able to have HT for any menopausal urinary symptoms such as women with breast cancer. For symptoms of vaginal atrophy, they can use vaginal moisturizers for normal relief and vaginal lubricants to relieve dryness prior to intercourse.
Non-hormonal treatments for bladder control symptoms, including those related to pelvic organ prolapse and weakening of the pelvic floor muscles, can involve lifestyle changes and medical procedures. These include:
- Reducing caffeine
- Bladder-training techniques that increase the capacity to hold urine, control the timing of urination, and control body functions with the help of a machine
- Maintaining a healthy weight
- Avoiding stress to the pelvic area and doing Kegel exercises
- Electrical stimulation of the bladder muscles
- A device placed in the urethra that blocks leakage
- Various surgical techniques to restructure support for the prolapsed organ.
Read Also: How Does A Urinary Tract Infection
Herbal Remedies And Vitamins
No herbal remedy has been proven to treat or prevent a UTI, and not all are tested for safety, so its best to discuss any herbal treatments with a healthcare professional first.
There are some herbal supplements that may have anti-inflammatory and anti-bacterial properties that can be helpful in treating UTI symptoms.
Studies have shown that certain herbal supplements, like garlic extract, have strong anti-inflammatory properties and may help reduce the growth of bacteria, including E. coli.
Other natural supplements like D-mannose, a sugar naturally found in foods like cranberries and apples, may have antibacterial properties which can help relieve UTI discomfort. Both can be taken in the form of a capsule.
Cranberry extract or cranberry juice or a vitamin C supplement may also help a UTI go away faster by changing the pH balance of your urine to help keep bacteria from growing.
While not proven to treat a UTI, these may help you feel better faster.
Treatment Of Contributing Factors
Vaginal atrophy is common in postmenopausal women and can be identified on pelvic examination by the appearance of dry, friable, and thin mucous membranes. The pathogenesis of recurrent UTIs is believed to be due to alterations in bacterial flora, changes in vaginal pH, and breakdown of natural mucosal barriers preventing ascending infection. The mechanism of local estrogen replacement stimulates blood flow, increases pH, and aims to restore mucosal barriers. A Cochrane review from 2008 cited two randomized clinical trials showing that vaginal estrogens reduced the recurrence of UTIs compared to placebo with RR of 0.25 and 0.64 in each study . No such benefit was found with oral estrogens.
In our practice, if there is evidence of vaginal atrophy on pelvic examination, we strongly consider such an approach. The risks for local therapy are very low, with the most common side effect being local irritation.
Preventive strategies
The most compelling evidence is for use of intravaginal suppositories of Lactobacillus crispatus. In a recent RCT, use of such an approach had a relative risk of 0.50 in young women . Given the low risk-benefit profile of intravaginal suppositories taken on a weekly basis after treatment of the acute UTI, this tends to be an attractive option for patients interested in non-antibiotic-based approaches. If intravaginal Lactobacillus suppositories are not available at a retail pharmacy, patients may be directed to online retailers such as Amazon.
Recommended Reading: How Can A Woman Get A Urinary Tract Infection
Classification Of Urinary Tract Infections
UTIs are classified into 6 categories. The first category is an uncomplicated infection this is when the urinary tract is normal, both structurally and physiologically, and there is no associated disorder that impairs the host defense mechanisms. The second category is an complicated infection this is when infection occurs within an abnormal urinary tract, such as when there is ureteric obstruction, renal calculi, or vesicoureteric reflux. The third category, an isolated infection, is when it is the first episode of UTI, or the episodes are 6 months apart. Isolated infections affect 2540% of young females. The fourth category, an unresolved infection, is when therapy fails because of bacterial resistance or due to infection by two different bacteria with equally limited susceptibilities. The fifth category, reinfection, occurs where there has been no growth after a treated infection, but then the same organism regrows two weeks after therapy, or when a different microorganism grows during any period of time., This accounts for 95% of RUTIs in women. Bacterial persistence happens when therapy is impaired by the accumulation of bacteria in a location that cannot be reached by antibiotics, such as infected stones, urethral diverticula and infected paraurethral glands. The sixth category, relapse, is when the same microorganism causes a UTI within two weeks of therapy however, it is usually difficult to distinguish a reinfection from a relapse.
Newer Concepts In The Prevention And Treatment Of Utis
The oral immunostimulant, OM-89, is an extract of 18 different serotypes of heat killed uropathogenic E. coli, which stimulates innate immunity by increasing neutrophils and macrophage phagocytosis. OM-89 shows promise in the prevention of recurrent UTIs .
A similar concept is provided by the vaginal vaccine, Urovac: it contains 10 heat killed uropathogenic bacteria including 6 different serotypes of UPEC, and 1 strain each of Proteus vulgaris, Klebsiella pneumoniae, Morganella morganii and
You May Like: What Causes Urinary Tract Infection In Women
Consider Adding Some Cranberry To Your Diet
Research supports the benefit ofcompounds found in cranberries, known as proanthocyanidins , for reducing the risk of getting a UTI. If given a chance, bacteria that enter the urinary tract will attach themselves to the inside surface of the bladder wall.
Studies have shown that it takes36 mg ofproanthocyanidins to help fend off bacteria from sticking to your bladder wall before they have a chance to hang around and cause an infection. You can get this level of PACs in 8-10 oz of 27% cranberry juice, 1 ½ cups of fresh cranberries, ½ cup of cranberry sauce, and 1 ounce of sweetened dried cranberries.
You May Like: Cranberry Supplements For Urinary Tract Health