Getting Help For Overactive Bladder
The first step in treatment is to ask for help. It may feel funny talking to your doctor about something as private as urinary issues, but rest assured that your doctor is a professional and is here to help. Be prepared before your appointment by keeping a bladder diary for a few days. This will help your doctor see the extent of your problem, and may help him or her to see any triggers that may be causing your urinary urgency issues.
Be prepared to have a thorough discussion with your doctor about your overactive bladder symptoms, as well as any other symptoms you may be experiencing. You should also let you doctor know if you suffer from any other conditions, such as diabetes, and provide a list of medications youre currently taking, which may be contributing to your symptoms.
Making a list of questions beforehand is also a great idea to ensure that you dont forget anything during your appointment. You may want to ask your doctor about different treatment options that he thinks may be a good fit for you, or about any options youve read about that youre interested in trying. Make sure you find out about the potential side effects for any treatment your doctor proposes, as well as what you can expect in terms of a success rate.
Dont Miss: Can You Have Intercourse While Having A Bladder Infection
Impact On Quality Of Life
OAB significantly impairs QoL, increases depression scores, and reduces quality of sleep. OAB that involves urgency incontinence is associated with the most severe impairment. Persons with OAB who have poor sleep quality report chronic fatigue and difficulty performing daily activities. An increased number of hip fractures due to falls in elderly persons have been attributed to OAB because of the nocturia component. Many such falls involve the individual tripping or losing balance while getting out of bed.
Individuals with OAB develop coping strategies to manage or hide their problems . These coping strategies, along with the OAB symptoms themselves, commonly affect interactions with friends, colleagues, and families and thereby have an adverse impact on QoL.
Notable psychological effects of OAB and urinary incontinence include fear, shame, and guilt. In elderly people with OAB and incontinence, the need for assistance with toileting, shopping for protective undergarments, and laundry may place an additional burden on family members.
Worries and concerns regarding odor, uncleanliness, and leakage during sexual activity may lead individuals to refrain from intimacy. Frequent urination and the need to interrupt activities may affect the persons work and ability to travel. Studies of the impact of OAB and urinary incontinence demonstrate decreased levels of social and personal activities, increased psychological distress, and an overall decrease in QoL.
References
Can Menopause Cause Urinary Incontinence Or Bladder Control Issues
The chances for urinary incontinence generally increase with age. As we get older, the muscles supporting the urethra and bladder naturally grow weaker, which can make it harder to hold urine in, allowing urinary leakage.2
Menopause can exacerbate the condition, since declining levels of the hormone estrogen can cause the lining of the urethra the tube that sends urine from the bladder out of the body to become thinner.3
Together, these two factors can add up to a greater likelihood that a woman will experience urine leakage and bladder control issues during perimenopause or menopause.
Also Check: What Causes Urinary Infections In Cats
What Is Urinary Incontinence
Urinary incontinence, or UI, is a common, and often embarrassing, condition in which patients can not prevent urine from leaking from their bladder. The severity can range from occasionally leaking urine when you cough or sneeze, to having an urge to urinate that is so strong you are not able to make it to a toilet in time.
Though this condition is mostly seen in patients as they get older, UI isnt an inevitable consequence of aging. UI is the result of a person losing control over their urinary sphincter, due to it being lost or weakened. There are five different types or urinary incontinence:
- Stress incontinence: when leaks are caused by pressure on the bladder due to coughing, sneezing, laughing, or exercising.
- Urge incontinence: having sudden, intense urges to urinate followed by the involuntary loss of urine.
- Overflow incontinence: the frequent and constant dribble of urine due to the bladder not fully emptying.
- Functional incontinence: a physical or mental impairment that keeps you from making it to the bathroom on time.
- Mixed incontinence: when you experience multiple types of urinary incontinence.
Urge Incontinence And Overactive Bladder
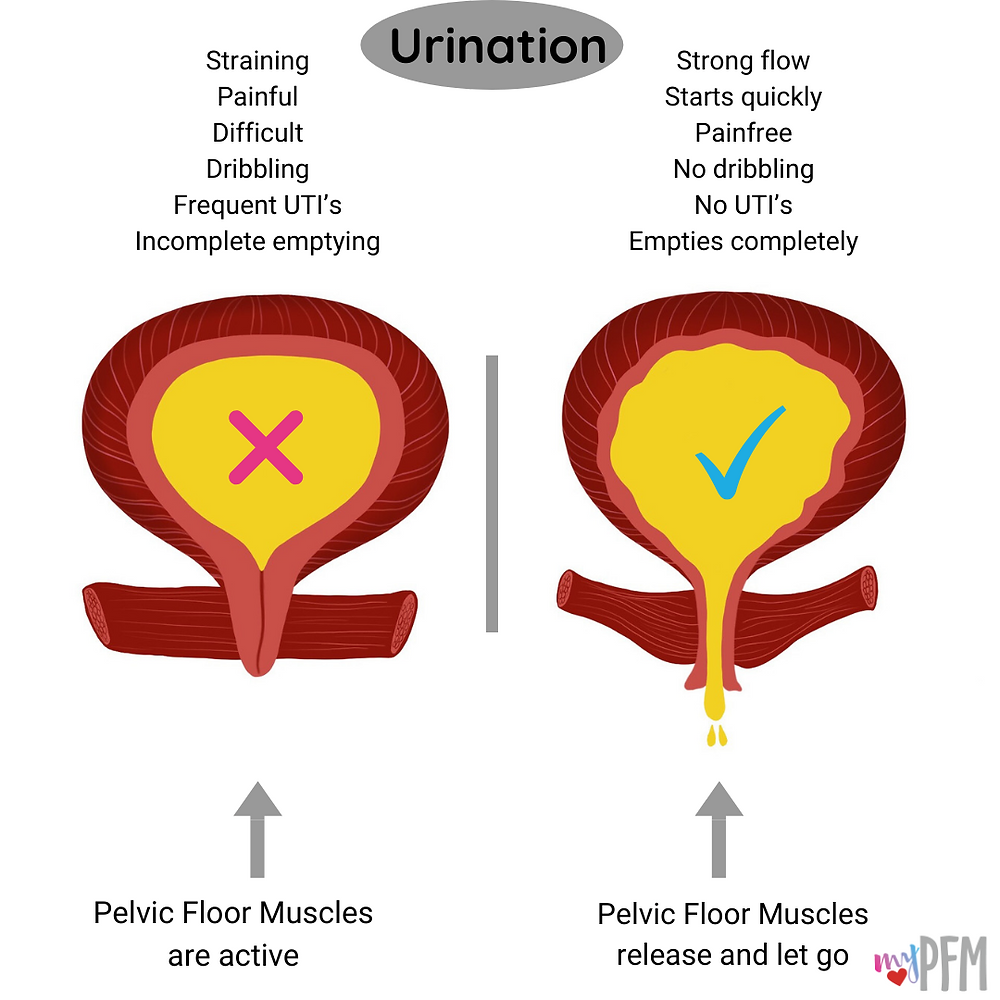
As your bladder fills up, your brain sends a signal to tighten the muscles of the pelvic floor and urethra. These muscle contractions close the urethra to help hold urine in the bladder. Once your bladder feels full, it sends a signal back to the brain. If you are ready to go to the bathroom, the brain responds with a signal that releases the muscles and allows urine to flow from the bladder, through the urethra and out of the body.
Your brain, bladder and muscles in the urinary system are supposed to work together to control the flow of urine. When you have urge incontinence or an overactive bladder, some part of this circuit breaks down.
An overactive bladder is when strong urges prompt you to go the bathroom more often than normal. Urge incontinence is when the urges associated with an overactive bladder prevent you from holding back urine before you get to the bathroom.
If you find that you are going to the bathroom frequently, your bladder muscles might be contracting before your brain is ready to allow it. Or your brain might be sending signals at the right time, but your muscles might be too weak or uncoordinated to function properly. If you just have a strong urge to urinate, there might be a problem with the nerves that your brain uses to transmit the signals.
A small percentage of people with neurological conditions, such as Parkinsons disease or a history of strokes, are prone to these conditions. Certain medications also can cause overactive bladder.
Recommended Reading: Urinary Tract Infection Treatment Amoxicillin
Molecular Basis For Plasticity Due To Ngf: Sodium Channel Isoforms
How could NGF produced by a target tissue, as in SCI, obstruction, and inflammation, and then retrogradely transported to the DRG lead to OAB? Recent data suggest that membrane conductance and thus excitability of DRG neurons are altered in models associated with increased access to NGF. This altered conductance is postulated to result from changes in the structure or combination of protein subunits of sodium and potassium channels in the cell membrane. A change in Na+ channel isoform appears sufficient to change the properties of afferents. NGF is known to lower the threshold for firing of bladder neurons and induce spontaneous and burst firing .23 The site of abnormal ectopic firing has been determined to be the DRG, and the firing appears to be due to changes in the isoforms for voltage-gated Na+ channels, which causes spontaneous ectopic discharges. Voltage-gated Na+ channels generate currents during the upstroke of the nerve action potential and are involved in the propagation of the nerve impulse.
TTX binds to and inactivates voltage-gated Na+ channels. Most voltage-gated Na+ channels exhibit rapid inactivation kinetics and sensitivity to nanomolar concentrations of TTX. These Na+ channels are termed TTX-sensitive . Small bladder sensory neurons in the L6-S1 DRG show two types of Na+ currents, a rapidly inactivating TTX-S sodium current and a slowly inactivating TTX-resistant INa.
Overactive Bladder Vs Urinary Incontinence: Whats The Difference
Overactive bladder is a condition in which the bladder no longer has enough capacity to store pee. If you have an overactive bladder, you may have frequent urges to urinate or have incidents. When you lose control of your bladder, this is called urinary incontinence. Its a symptom rather than a disease. Incontinence can be the result of anything as simple as drinking too much water. Also, it can be a sign of something more serious such as a urinary tract infection .
You May Like: Life Seasons Urinari X Reviews
Treatments For Urinary Incontinence During Menopause
Urinary incontinence may be common after menopause, but its not something you have to live with. Depending on your symptoms and personal preferences, urinary incontinence can be treated with lifestyle changes, medication, surgery, or a combination approach.
To find the right strategy for addressing your bladder issues, start by talking with your healthcare provider. While bringing up urinary leakage can be uncomfortable, your healthcare provider can be an ally for finding effective, personalized solutions. Youre not alone in this incredibly common complaint, says Dr. Dweck.
For many women, incorporating bladder control exercises that work to strengthen the pelvic floor, may help. More specifically, Kegel exercises are an effective way to strengthen the pelvic floor muscles and help to regain bladder control. Giving the bladder more pelvic floor support can help prevent urinary leakage as well as provide other benefits, like more satisfying sex and preventing pelvic organ prolapse. Experts recommend performing Kegels on an empty bladder and working up to five sets of 10 repetitions per day.5
In some cases, low-dose topical estrogen creams can be helpful. For urge incontinence in particular, Botox injections can also be used to encourage overactive bladder muscles to relax.7
Resources
Does Overactive Bladder Only Happen In Women
More women than men experience overactive bladder, however, around three to 11 percent of men may experience urinary incontinence. The most common type of incontinence in men is urge incontinence, accounting for about 80 percent of cases. In men, stress incontinence can occur and may happen after prostate surgery, trauma or neurologic damage. With both women and men, the incidence increases with age.
You May Like: What Is Urinary Bladder Cancer
Overactive Bladder And Urge Urinary Incontinence In The Workplace
Any discussion of the effects of OAB and urge urinary incontinence in younger women has to consider the effects of these disorders in the workplace. Incontinence in working-age women has genuine economic consequences. Fultz and colleagues27 conducted a mail survey of women born in 1947 or earlier to assess their time use and activity patterns, including time spent at work. Incontinent women reported significantly fewer hours working for pay than did continent women. The median number of hours
Written byDr. Victor MarchionePublished onApril 30, 2016
Overactive bladder, or OAB, affects about 15 percent of the North American population. People who have OAB find themselves using the bathroom eight or more times a day and can even have urge incontinence involuntary loss of urine. Although it may appear that the older we get, the odds of us developing OAB increase, it really is not age-related. OAB occurs when contractions of the detrusor muscle within the wall of the bladder occur involuntarily. This, in turn, leads to more frequent trips to the bathroom.
Incontinence And Overactive Bladder
Millions of men and women suffer from bladder control issues, often called overactive bladder . Urinary incontinence, or difficulty controlling your bladder, is one of the most common types of OAB conditions.
Blessings urology specialist provide compassionate care and the latest treatments for all conditions related to overactive bladder, including incontinence.
Recommended Reading: Chronic Urinary Tract Infection In Elderly
What Are The Symptoms Of Urge Incontinence And Overactive Bladder
Urge incontinence and overactive bladder can occur at any time and often without warning. You might have one or both of these conditions if you:
- Have the urge to urinate so severely that you leak before you reach the bathroom.
- Go to the bathroom frequently to avoid leaks.
- Feel the urge to urinate while washing dishes, putting your key in the door, pulling into your driveway or having sex.
- Get up frequently from sleeping to urinate.
- Make sure you know the location of bathrooms during your daily activities.
- Limit activities out of concern about leaks or an inability to find a bathroom when you need one.
- Avoid going to the beach or wearing light-colored clothing because of leaks or fear of leaks.
- Feel afraid or ashamed to discuss this problem.
A Mixed Case Of Overactive Bladder & Urinary Incontinence
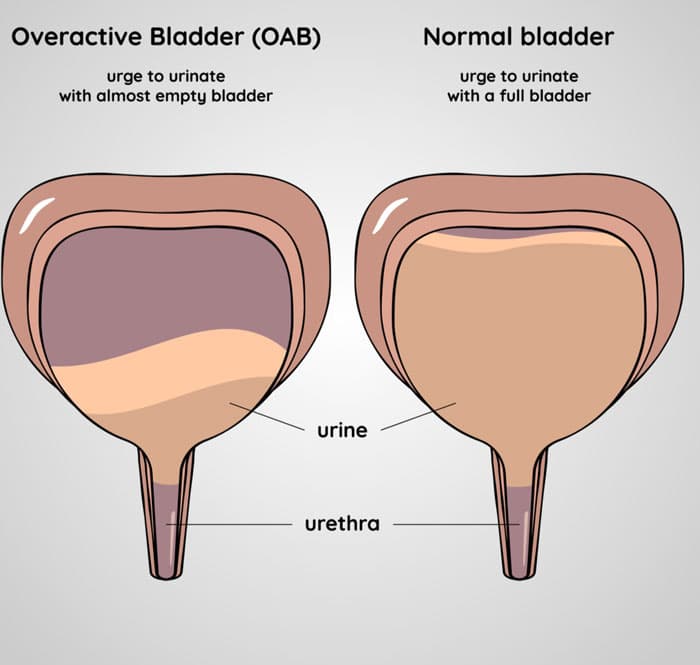
The reason for urinary incontinence and an overactive bladder is the involuntary passing of urine. As a result, unless a professional urologist performs extensive investigation, it can be impossible to discern between the two. The good news is that you can manage both conditions using adult diapers and pull-ups.
Recommended Reading: Canine Urinary Tract Infection Symptoms
Botox Injections In The Bladder
An option for women who have failed all other medications. Onabotulinum toxin A is injected into the bladder muscle and causes partial paralysis of the detrusor muscle. Each course last approximately 6-12 months and patients typically will require multiple top-ups for the botox to be effective . This is performed under sedation in hospital as a day case and the botox takes approximately 7-10 days before working.
The botox is injected into the bladder wall as shown in the image, thru a small cystoscope that is introduced via the urethra. Approximately 5% of women will have trouble emptying there bladder following botox and use of a temporary catheter would then be required. The botox is now funded on the PBS in Australia when administered by a Urogynaecologist.
What Are The Symptoms Of Overactive Bladder
Overactive bladder represents a collection of symptoms. These symptoms include:
- Urinary urgency. Urinary urgency is a sudden, uncontrollable need to pee. Once you feel the need to pee, you have a short amount of time to get to a bathroom.
- Frequent peeing. A frequent need to pee means you have to go to the bathroom more often than usual.
- Urge incontinence. Urge incontinence is a sudden, uncontrollable need to pee, and you may leak pee.
- Nocturia. Nocturia is the need to get up to pee at least two times each night.
You May Like: Urinary Tract Infection Blood In Pee
How Do I Control Urges When Resetting My Bladder
Controlling your urges is a key step in resetting your bladder. The following strategies may help:
- Stop what youre doing and stay put. Stand quietly or sit down, if possible. Remain as still as possible. When youre still, its easier to control your urges.
- Squeeze your pelvic floor muscles quickly several times . Dont fully relax in between Kegels.
- Relax the rest of your body. Take several deep breaths to help you let go of any tension.
- Concentrate on suppressing your urge to pee.
- Wait until the urge goes away.
- Walk to the bathroom at a normal pace. Dont rush. Continue squeezing your pelvic floor muscles quickly while you walk.
Patience is important. Retraining your bladder usually takes at least six to eight weeks to see results. Talk to a healthcare provider if you have any questions or arent happy with your progress. They may prescribe medications for you to take while youre resetting your bladder to help you achieve the best outcome.
Adult Pediatric Urology & Urogynecology
The attentive, compassionate physicians, providers, and staff at Adult Pediatric Urology & Urogynecology are committed to providing innovative, quality patient care in our state-of-the-art facility.
From screening and prevention to treatment and recovery, we will be there for you. Our team of dedicated physicians has been serving residents of Nebraska, Iowa, and South Dakota for more than 25 years.
Donât Miss: New Drug For Overactive Bladder
Also Check: Best Juice For Urinary Tract Infection
Managing Bladder Or Urinary Incontinence
Sometimes urinary incontinence can last a short time, depending on whatâs causing it. But sometimes incontinence can be long-term and uncomfortable, making some everyday activities difficult to manage.
Your health care team will ask you questions to determine the type of bladder incontinence you might have. Then, you might need tests to verify the type and learn the cause of it which will help them know the best way to manage it.
- Pelvic floor muscle strengthening may be recommended. A physical therapist that specializes in pelvic floor muscle exercises can help. This might help muscle strength and bladder control get better by doing exercises that tighten and relax muscles that control the flow of urine.
- Bladder training canhelp manage how often you need to urinate throughout the day, by assigning certain time intervals to empty your bladder.
When To Consult A Doctor
If you notice a sudden change in your bathroom habits, have issues holding urine, feel an ever-present urge to urinate, visit bathroom more than eight times in a day, or have trouble urinating you might want to set up an appointment with your doctor to get things checked out. Your doctor might also be able to help you have a neurogenic bladder diagnosis better.
You May Like: Augmentin For Urinary Tract Infection
Who Does Overactive Bladder Affect
Overactive bladder is most common in people 65 and older. Women may have OAB at a younger age, usually around 45.
How common is overactive bladder?
Overactive bladder is common. It affects up to 33 million adults in the U.S., including as many as 30% of men and 40% of women. However, that number may be higher because many people may feel embarrassed and wont get help.
How does overactive bladder affect my body?
Overactive bladder symptoms can cause stress and affect your quality of life.
Wet Overactive Bladder Vs Dry Overactive Bladder: Whats The Difference
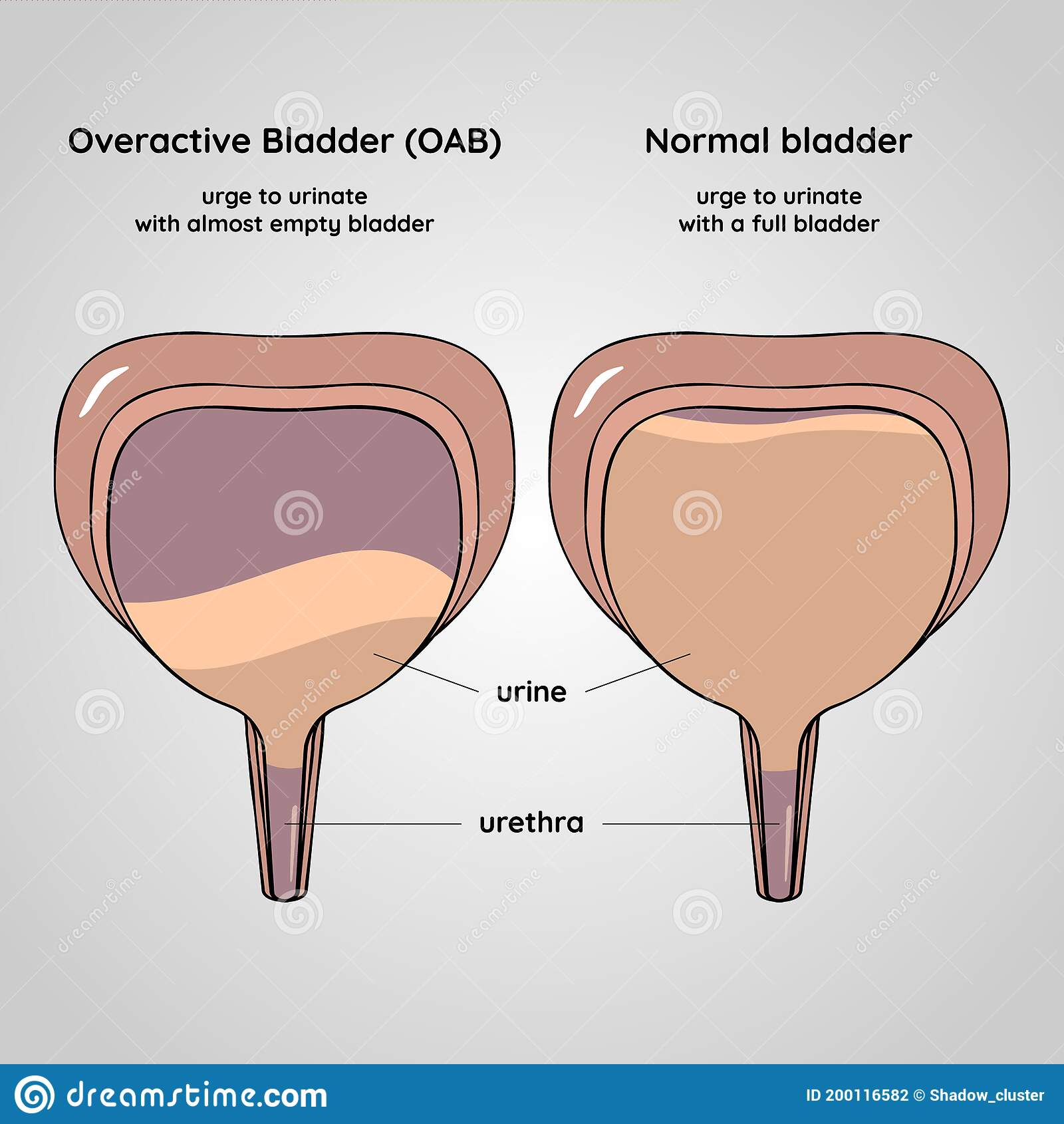
Dry type is when you have urgency where you really have to go to the bathroom and its difficult to wait, but you dont leak, and then theres wet type, where you also have the really strong urge but you cant make it to the bathroom in time and do have urine leakage, says Wu.
If you have both of those kinds, its called mixed, she adds.
Don’t Miss: Holding Pee Urinary Tract Infection