Managing Urinary Incontinence Due To Prostate Cancer
Recently there has been a lot of progress in dealing with urine leakage. There are many ways of managing the problem.
If urine leakage becomes a long term problem, discuss this with your doctor or nurse. They can help or can refer you to a specialist incontinence clinic. Staff there can help you with muscle exercises, bladder training and medicines.
Current Management Of Post
- 1Urology Department, Uniklinik RWTH Aachen, Aachen, Germany
- 2Maastricht University Medical Center , Maastricht, Netherlands
- 3Bucharest University Emergency Hospital, Bucharest, Romania
- 4Division of Oncology, Unit of Urology, Urological Research Institute, IRCCS Ospedale San Raffaele, Milan, Italy
- 5Mainz University Hospital, Mainz, Germany
How Common Is Urinary Incontinence After Prostate Surgery
If you have a radical prostatectomy, a tube called a catheter will be placed inside your bladder to allow urine to drain. When the catheter is removed, most men will have some difficulty controlling their urine flow.
For most men, the urinary leakage will improve in the months following surgery. In an NHS trial, 46% of men needed to use absorbent pads six months after having a radical prostatectomy. But, one year on from having the procedure, this figure had improved to 17%.
Recommended Reading: What Can Happen If A Urinary Tract Infection Goes Untreated
What If These Treatments Do Not Work
If these interventions do not work, you may be referred to a urologist for additional tests on your bladder and sphincter. These tests will determine what type of incontinence you have, how well your bladder is working, and what other treatments might be best for you. This often involves a urodynamic test and a cystoscopy. Both of these procedures are performed in the office, usually during the same visit. They provide your urologist with specific information to help find which procedure might be best for you.
The urodyamics test involves placing a very small catheter in your bladder. This catheter fills the bladder with fluid and measures bladder activity and pressure during filling and voiding . You will also be asked to cough and strain so your provider can see if and how easily you leak urine.
A cystoscopy may also be performed to look at the urethra, the anastomosis , and the bladder. After these tests, your provider will go over the results with you and recommend which treatments are best suited for your condition.
Recommended Reading: Does Enlarged Prostate Affect Ejaculation
‘just Cant Wait’ Card
You can get a card to show to staff in shops or pubs etc. It allows you to use their toilets, without them asking awkward questions. You can get the cards from Disability Rights UK or the Bladder and Bowel Community. They also have a map of all the public toilets in the UK.
You could get a key to disabled toilets if you need to access them quickly. You buy the RADAR key from Disability Rights UK. But this should only be used by people who need quick access to a disabled toilet due to a disability or medical condition.
You May Like: Symptoms Of Pinworms In Urinary Tract
Problems After High Intensity Focused Ultrasound
Youre more likely to get urinary problems after HIFU if youve already had other treatments for prostate cancer. Possible urinary problems include:
- difficulty urinating
- urine infections.
Difficulty urinating
HIFU usually causes the prostate to swell for a week or two, so youll have a catheter to drain urine from your bladder until the swelling has gone. HIFU can also cause the urethra to become narrow, making it difficult to empty your bladder .
Leaking urine
HIFU can cause some men to leak urine when they cough, sneeze or exercise . This may be more likely if youve already had radiotherapy. There are ways to manage leaking urine.
Urine infections
Some men get a urine infection after HIFU. If this happens, youll be given a course of antibiotics to clear the infection.
Why Does It Happen
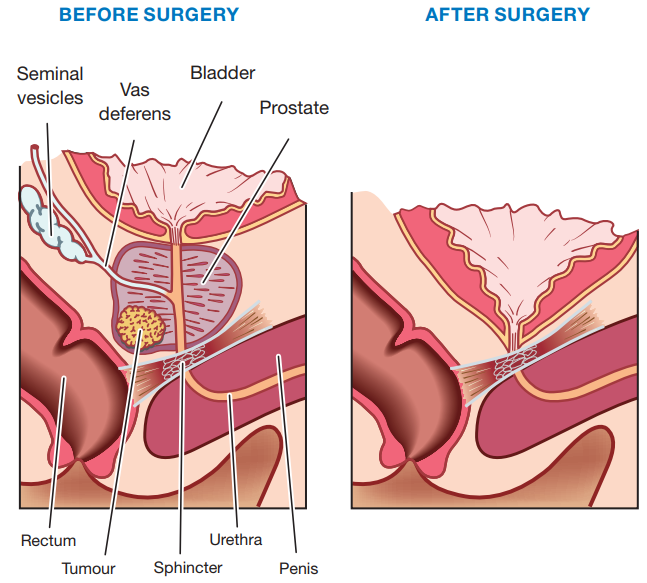
- At the point where the bladder and urethra join, there is a ring of muscles known as the bladder neck sphincter, which opens and closes like a camera shutter. The bladder neck sphincter is closed most of the time to prevent urine leaking out, but when it gets a signal from the brain, it opens to allow urine to be passed.
- If the bladder neck sphincter is damaged during prostate cancer surgery, this can lead to urinary incontinence.
- Another sphincter is part of another set of muscles below the prostate called the pelvic floor. These muscles are also involved in bladder control.
Most men regain their bladder control over time and are fully recovered within 6 to 12 months. It is important to get professional advice to help cope bladder weakness during this time.
You May Like: Pomegranate Juice For Urinary Tract Infection
Over The Counter For Bladder Control
So, whats available to men OTC for bladder control?
For incontinence care at home, there’s a device called a Cunningham Clamp that can be used very temporarily, says McCormick. It’s just a soft clip that stays on the penis and can help hold back urine. The user decides when to remove it, to relieve themselves.
The bladder is supported by pelvic floor muscles, so in some patients stress incontinence can be improved by simple light pelvic exercises to restore flexibility and muscle strength. McCormick says Its also helpful to drink enough water and avoid caffeine and alcohol.
How Do You Retrain Your Bladder After A Catheter Is Removed
Gradually increase the amount of time between bathroom breaks. Delay urination. When you feel the urge to urinate, hold it for another five minutes or so. Then gradually increase the amount of time by 10 minutes, until you can last for at least three to four hours without having to go to the bathroom.
You May Like: Does Enlarged Prostate Affect Ejaculation
Recommended Reading: Common Urinary Tract Infection Antibiotics
Expected Sequence Of Return To Continence
From my readings and experience the sequence of return to continence will be: while standing, while walking on a flat surface, while walking uphill, while walking downhill, while running and while playing tennis, while coughing and sneezing. There is a significant improvement when one reaches the next stage but it one doesnt reach 100% continence at that stage. Instead, there are phases of return to continence, such as initially 20 percent continence while standing/ walking, then 90 percent, and so on. Some minor leakage will occur in previous stages for a few weeks till the body masters these earlier stages.
Note, for the latter, also include yawning. Big yawnscan prompt leakage. Addendum 20 April 2018: Finally, I have found that while control is getting better even while sneezing, etc., there is one posture which seems to open up the sphincter. Obviously I dont do such extreme backward bend, but even a bit of this type of bend still remains to be overcome. Posture illustrated below .
Addendum 18 May 2018: Leaks are continuing in odd postures, e.g. while bending forward while standing near a hand dryer. Also while bending backward . And when bladder is full while getting up from bed.
- slides here. At three months Im mostly continent while walking uphill.
Also Check: Does Enlarged Prostate Affect Ejaculation
How To Minimize Urinary Incontinence After Prostate Surgery
Obese men are at a significantly greater risk of experiencing urinary incontinence post surgery. Prior to surgery, Dr. Samadi encourages obese men to undergo an aggressive weight loss regimen to optimize their readiness for surgery and recovery. Kegel exercises are recommended for all men to strengthen the urinary sphincter muscles. The exercise is performed in repetitive sets of clenching the muscle that stops urine flow. There is a significant benefit to beginning them prior to surgery and then continuing the exercise routine post operatively.
Men experiencing longer-lasting incontinence issues have a range of treatment options, including collagen injections and even surgery. Longer-term incontinence issues must be addressed, as left untreated they can lead to isolation and depression. Dr. Samadi knows that urinary control and sexual potency are of utmost importance to men recovering from prostate cancer. All patients receive ongoing, compassionate and practical assistance after surgery to help them achieve optimal urinary and sexual function performance.
Also Check: Azo Urinary Tract Defense Antibacterial Protection
What If The Incontinence Does Not Improve Or Is Bothersome
If you have a bothersome amount of incontinence or if it does not improve with the above measures, many men will benefit from seeing an incontinence practitioner. There is a wide range of treatments available.
Once you decide to see an incontinence practitioner, be prepared to answer questions regarding the type of symptoms you are having, the number and type of pads you might be using, and previous treatments you have had for prostate cancer and for incontinence. You should be honest about how much the incontinence bothers you, and how willing you are to have additional treatments, potentially including surgical procedures.
During your first visit, the incontinence specialist will take your history and perform an exam. You will likely be asked to give a urine sample to rule out infection or blood in the urine. A bladder scan is often done in the office to see if you are completely emptying your bladder when you urinate.
The incontinence specialist will likely discuss more conservative treatments at first. A more rigorous pelvic floor exercise program might be recommended. You may also be given a biofeedback machine that allows you to see how strong your pelvic floor muscles are. The specialist may also discuss various medication therapies.
Points To Take Into Consideration After A Prostate Surgery

- Do not sit on hard floors.
- Avoid getting constipated.
- Consume at least 3 liters of water per day.
- Regularly use the drugs prescribed by your doctor.
- Do not drive for the first week during the recovery period after surgery. In addition, stay away from activities such as cycling, exercising, and horseback riding for 6 months, which may strain the groin area.
- Do not wear trousers that tighten the groin area.
- Do not consume drinks that contain alcohol and caffeine.
- Do not shower in a sitting position after the surgery, unless your doctor tells you otherwise.
You May Like: Can An Iud Cause Urinary Tract Infections
Incontinence After Prostate Surgery: A Guide To Recovery And Care
After Linwood Wright, 68, of Danville, Va., had his prostate removed following a diagnosis of prostate cancer, he experienced incontinence that he thought would eventually clear up on its own. Although it did get better, now, five years after his surgery, he is still dealing with what he terms a “minimal” problem with bladder control.
Wrights case is not uncommon, as incontinence is a frequent side effect of prostate surgery. However, according to Dr. Judd Moul, director of the Center for Prostate Disease Research in Washington, D.C., in most cases it lasts only a few weeks. Occasionally, though, it may linger, leaving the patient to manage a permanent case of incontinence.
A Prostate Primer
Many prostate conditions can cause bladder weakness or other urinary problems in men. This is because the prostate gland surrounds the urethra, which is the tube that carries urine through the penis. Until puberty, the prostate is the size of a small marble, but after puberty it gradually grows to about the size of a golf ball. After about age 50, the prostate begins to grow again.
Sometimes this growth doesnt cause any problems at all. However, in some men, the prostate enlarges to the point that it acts as a “clamp” against the urethra, resulting in symptoms such as difficulty starting urination, frequent urination or incontinence. If the problems become severe enough, surgery may be required to correct them.
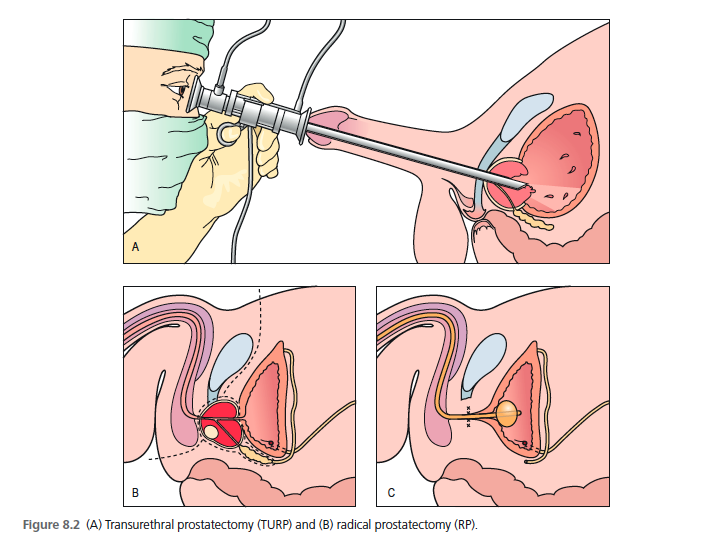
Prostate Surgery
Managing Incontinence
The Bigger Picture
Peer Review And Document Approval
An integral part of the guideline development process at the AUA is external peer review. The AUA conducted a thorough peer review process to ensure that the document was reviewed by experts in the treatment of IPT. In addition to reviewers from the AUA PGC, Science and Quality Council , and Board of Directors , the document was reviewed by representatives from AUA and SUFU as well as external content experts. Additionally, a call for reviewers was placed on the AUA website from January 14-28, 2019 to allow any additional interested parties to request a copy of the document for review. The guideline was also sent to the Urology Care Foundation to open the document further to the patient perspective. The draft guideline document was distributed to 49 external peer reviewers. All peer review comments were blinded and sent to the Panel for review. In total, 33 reviewers provided comments. At the end of the peer review process, a total of 476 comments were received. Following comment discussion, the Panel revised the draft as needed. Once finalized, the guideline was submitted for approval to the AUA PGC, SQC and BOD as well as the governing bodies of SUFU for final approval.
You May Like: Tips For Urinary Tract Infection
Predicting Urinary Incontinence After Radical Prostatectomy
Damage to the urethral sphincter complex, the surrounding structures, or their innervation leads to higher rates of urinary incontinence after rPR. In addition, certain biological factors and parameters known preoperatively, including older age, higher BMI, pre-existing LUTS, lower motor unit lesion, and functional bladder changes, have been identified to have a negative impact on continence rates after rPR .
Recently, a preoperative model was presented to predict incontinence before rPR . According this nomogram, high risk for biochemical recurrence, adjuvant radiotherapy, lower results in the validated quality of life questionnaire EORCT QLQ-C30/QoL, higher sum score of the validated questionnaire International Consultation of Incontinence QuestionnaireâUrinary IncontinenceâShort form and higher patient age, were associated with statistically significant higher sum scores of the 12-month ICIQ-UI-SF, thus, representing higher impact of urinary incontinence . Together with the preoperative model a new, postoperative nomogram was introduced to inform patients about the probability of an additional surgery for incontinence or, on the other hand, about the importance of enduring with a strict pelvic floor muscle training protocol .
Interestingly, these results did not show any association with ICIQ-UI-SF, when including surgery volume .
Practice Good Toilet Habits
Go to the toilet when your bladder feels full dont get into the habit of going just in case. After prostate surgery you may find that you do not experience the sensation of a full bladder. The sensation of a full bladder will gradually return as you are able to hold on longer. It is important to practice holding on to increase the amount of urine your bladder can hold.
Read Also: Hill’s Urinary Hairball Control
What Causes Incontinence After Prostate Surgery
Urinary incontinence is a potential side effect of prostate removal surgery. The prostate is located just below the bladder and surrounds the urethra. Removing it, or using radiation to treat it, can sometimes cause damage to the nerves and muscles of the bladder, urethra, and or sphincter, which controls the passage of urine from the bladder. This can result in urinary incontinence.
Arousal Incontinence A Concern After Prostatectomy
Arousal incontinence urine leakage when a man is sexually aroused – is common after radical prostatectomy, researchers report in the Journal of Sexual Medicine.
Radical prostatectomy is a frequent treatment for prostate cancer. After surgery, men might experience sexual issues, like erectile dysfunction and climacturia . However, less is known about arousal incontinence.
The research team sent questionnaires to 226 men who had undergone radical prostatectomy within the previous 24 months. The mens average age was 64 years.
Half of the men said they had had arousal incontinence at least once since their surgery. For most of the men, the problem started within the first three months after prostatectomy.
About 39% of the men were experiencing it at the time of the study. Eleven percent said theyd had arousal incontinence in the past, but no longer did. Among this second group, 50% said that the situation had gotten better within seven months.
About three-quarters of the men said physical stimulation led to arousal incontinence. For 25%, urine leakage happened when they were psychologically aroused, too.
Arousal incontinence didnt happen with every sexual encounter, however. For 57% of the men, it occurred less than half the time they were having sex. Most men said the amount was a tablespoon or less.
Jimbo, M., et al.
Prevalence of Climacturia in Patients with History of Definitive Therapy for Prostate Cancer
Don’t Miss: Nature’s Sunshine Urinary Maintenance
What Types Of Incontinence Can Happen After Rp
There are two main types of urinary incontinence after RP:
- Urgency incontinence is when you feel the need or urge to urinate but cannot make it to the toilet in time. This is often due to bladder spasms and medication can help. This type of incontinence is caused by changes in the way the bladder behaves after surgery.
- Stress urinary incontinence is leakage of urine with movement or effort and can happen when you cough, sneeze, lift something heavy, change position, or exercise. This type of incontinence may be caused by damage to your external sphincter muscle. Almost all men will have some degree of SUI right after their urinary catheter is taken out. A urinary catheter is placed short term to collect urine during and while recovering from surgery. You may be taught how to do pelvic floor exercises to help with urinary control.
What Kinds Of Surgeries Treat Urinary Incontinence After Your Prostate Is Removed
There are two types of surgery for urinary incontinence: the urethral sling and the artificial urinary sphincter. Usually, the incontinence needs to last for about one year after the prostatectomy to be sure there is not going to be further improvement before your healthcare provider suggests this type of therapy.
Read Also: Probiotics For Urinary Tract Infection