Control Your Urge To Urinate
You may be able to control, or suppress, the strong urge to urinate, which is called urge or urgency suppression. With this type of bladder training, you can worry less about finding a bathroom in a hurry. Some people distract themselves to take their minds off needing to urinate. Other people find that long, relaxing breaths or holding still can help. Doing pelvic floor exercises to strengthen your pelvic floor also can help control the urge to urinate. Quick, strong squeezes of the pelvic floor muscles can help suppress urgency when it occurs, which may help you get to the toilet before you leak.
Why Does Pregnancy Cause Incontinence
During pregnancy, your body goes through a lot of physical changes. As your uterus stretches to hold the growing baby, a few things happen. Your bladder can be squished by the expanding baby, making your bladder hold less than before. You might experience an increased urgency to pee during pregnancy because your bladder cannot hold as much as before. This might become even more challenging towards the end of pregnancy when the baby is at its largest.
Another reason for incontinence during pregnancy is the weakening of your pelvic floor muscles. These muscles are the support structures for all of the organs in your pelvis. During pregnancy, they can be stretched and weakened as your uterus expands.
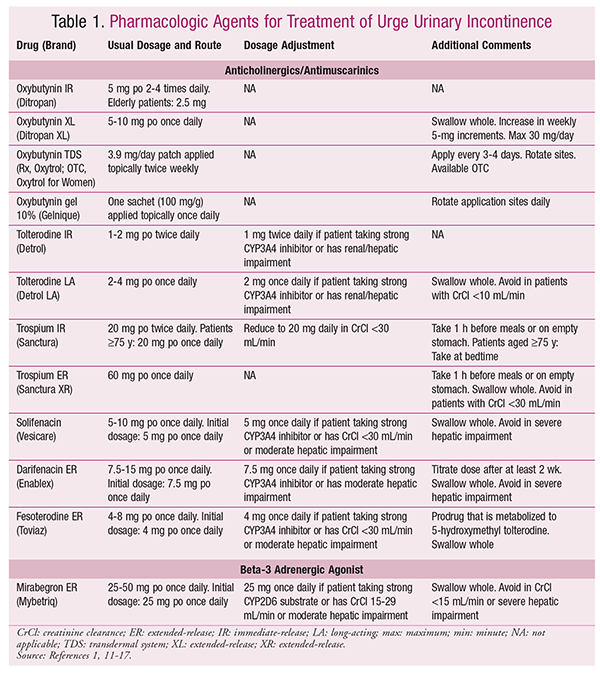
Drugs For Treatment Of Urinary Incontinence
teaserWalsgrave University Hospital of Coventry, UK
Vijay AnandYork House Medical Centre, UK
Urinary incontinence is a common, chronic condition which requires long-term management and is associated with significant negative impact on an individual. Medical management associated with conservative measures still plays an important role in its management. Surgery is still the mainstay treatment of stress urinary incontinence but it is not free from complications. When drugs are prescribed, long-term adherence to therapy is poor. Efforts to improve the clinical effectiveness of pharmacological therapies have included extended release formulations and alternative delivery mechanisms.
Malfunction occurring at various levels may result in bladder control disorders, which can be classified as disturbances of filling/storage or voiding/emptying. Failure to store urine may lead to various forms of incontinence , and failure to empty can lead to urinary retention, which may result in overflow incontinence. The disturbed function can be improved by agents decreasing detrusor activity, increasing bladder capacity and/or increasing outlet resistance.1 Several promising drug targets have been identified to improve the pharmacological treatment of UI.2
Drugs acting on membrane channelsAt present there is insufficient evidence to suggest that calcium channel blocking agents and potassium channel opening agents are effective in the treatment of DO.
Don’t Miss: Preventing Urinary Tract Infections In The Elderly
Treatment Of Urge Incontinence
The anticholinergic agents oxybutynin and tolterodine are used widely to treat urge incontinence. These medications are not, however, the most effective therapies. Behavior therapies are more effective, and theynot medicationsshould be first-line treatment.
Behavior Therapy
Behavior therapies for urge incontinence include bladder training and pelvic floor muscle exercises. Bladder training is more effective than oxybutynin and improves incontinence in more than 50 percent of patients.6 Kegel exercises are even more effective. In a randomized controlled trial 7 comparing Kegel exercises with oxybutynin in patients with urge incontinence, patients performing Kegel exercises had an 81 percent reduction in incontinence episodes compared with a 69 percent decrease in oxybutynin-treated patients, a statistically significant difference.
Although biofeedback commonly is used to help patients learn effective Kegel technique, evidence suggests that biofeedback training does not result in decreased frequency of incontinence episodes compared with Kegel exercises alone.8 Physicians should keep in mind that successful use of Kegel exercises is dependent on a patients motivation and ability to cooperate with the exercise routine.
Medications
When a single drug treatment does not work, a combination therapy such as oxybutynin and imipramine may be used. Although their mechanism of action differs, oxybutynin and imipramine work together to improve urge incontinence.
References
Incontinence Associated With Benign Prostatic Hyperplasia
Chronic bladder outlet obstruction leads to functional changes, such as decreased bladder compliance and detrusor overactivity. In turn, this may result in frequency, urgency and urgency incontinence.10Detrusor overactivity, mediated by M2 and M3 muscarinic receptors, contributes to lower urinary tract symptoms in approximately 15% of men.11
In patients with overactive bladder syndrome secondary to bladder outlet obstruction, treatment varies from watchful waiting to drug therapy and various surgical options depending on the severity of symptoms and indications for intervention.11The mainstay of drug treatment includes alpha adrenergic receptor blockers and 5-alpha-reductase inhibitors. If the overactive bladder syndrome is secondary to bladder outlet obstruction there may be a role for combinations of these drugs. Although there is a risk of acute urinary retention with alpha adrenergic receptor blockers and antimuscarinic drugs in combination, the rate is low.12
With 5-alpha-reductase inhibitors, common adverse effects include fatigue, loss of libido and ejaculatory and/or erectile dysfunction. Long-term use at the end of four years shows an absolute reduction in the overall risk of developing prostate cancer.13The alpha blockers can cause hypotension. As the elderly are more susceptible to orthostatic hypotension, they may have an increased risk of falls.
Also Check: How Does Cranberry Juice Help Urinary Tract Infections
Why Is Urinary Incontinence A Health Issue
Urinary incontinence is a very common problem in aging women . When women leak urine during exercise, sneezing, or coughing, doctors call this type of incontinence stress-related . When women have strong urges to urinate and have trouble holding urine until getting to the bathroom, they may have what is known as urgency incontinence . Although most women have one or the other type of incontinence, older women often have both types. Incontinence hurts women’s self-confidence, interferes with their ability to enjoy their favorite activities, and decreases the quality of their lives .
Other Bladder Control Medications
If symptoms of urinary incontinence are thought to be caused by an enlarged prostate, different medications can be offered to reduce these symptoms. The prostate gland wraps around the urethra , and if it is enlarged, it could squeeze the urinary passage tight, making the emptying of bladder more difficult and incomplete.
In brief, the following categories are available for the treatment of urinary symptoms caused by an enlarged prostate :
- Alpha-blockers, terazosin , doxyzosin , alfuzosin , silodosin , and tamsulosin , work by relaxing the muscles around the urethra and prostate, thus, making urination more comfortable and complete. These medications start to relieve symptoms within a few weeks, but they do not affect the prostate size.
- 5-alpha reductase inhibitors, finasteride and dutasteride , work by reducing the size of the prostate gland. They may take several months to become effective.
Recommended Reading: Urinary Urgency With Little Output
Medication To Treat Urinary Incontinence
One of the most common treatments for incontinence is medication. In some cases, medication is the best treatment for improved bladder control. Medication can also be an alternative to more invasive treatments like surgery, medical devices , interventional therapies , and catheters. There are three primary types of medications that treat incontinence.
Am I At A Higher Risk Of Incontinence At An Older Age
Your body constantly changes throughout your life. As you age, the muscles that support your pelvic organs can weaken. This means that your bladder and urethra have less support often leading to urine leakage. Your risk for developing incontinence as you age might be higher if you have a chronic health condition, have given birth to children, went through menopause, have an enlarged prostate or have had prostate cancer surgery. Its important to talk to your healthcare provider over time about the risks of incontinence and ways you can manage it without interference to your daily life.
You May Like: Urinary Tract Over Counter Medicine
Mechanisms Of Urinary Continence
In healthy individuals, the urinary bladder senses the volume of urine by means of distention. Distention of the bladder excites afferent A-delta fibers that relay information to the pontine storage center in the brain. The brain, in turn, triggers efferent impulses to enhance urine storage through activation of the sympathetic innervation of the lower urinary tract . These impulses also activate the somatic, pudendal, and sacral nerves.1
The hypogastric nerves release norepinephrine to stimulate beta3-adrenoceptors in the detrusor and alpha1-adrenoceptors in the bladder neck and proximal urethra. The role of beta3-adrenoceptors is to mediate smooth-muscle relaxation and increase bladder compliance, whereas that of alpha1-adrenoceptors is to mediate smooth-muscle contraction and increase bladder outlet resistance.1 The somatic, pudendal, and sacral nerves release acetylcholine to act on nicotinic receptors in the striated muscle in the distal urethra and pelvic floor, which contract to increase bladder outlet resistance.1
Efferent sympathetic outflow and somatic outflow are stopped when afferent signaling to the brain exceeds a certain threshold. At this point, the parasympathetic outflow is activated via pelvic nerves. These nerves release acetylcholine, which then acts on muscarinic receptors in detrusor smooth-muscle cells to cause contraction. A number of transmitters, including dopamine and serotonin, and endorphins are involved in this process.1
Outlet Factor Stress Incontinence
The most common storage dysfunction related to an outlet factor is stress incontinence. It is due to intra-abdominal pressure exceeding urethral closure pressure, causing involuntary loss of urine. If pelvic floor muscular training fails, the mainstay of treatment is surgery, although lifestyle modifications and controlling comorbidities which put chronic strain on the pelvis may have a supportive role.
Effective surgical options for stress incontinence include the synthetic mid-urethral sling and autologous fascial slings in women, and the transobturator bulbo-urethral sling in men. Implantation of an artificial urinary sphincter can be tried if sling surgery fails.
The role for drug therapy in stress incontinence is very limited. Duloxetine, which is a serotonin and noradrenaline reuptake inhibitor, has some effects on increasing bladder outlet resistance. It has been effective in controlling mild urinary stress incontinence in women,4 but it is not approved for this indication in Australia.
Also Check: What Is The Best Medicine For Urinary Tract Infection
Medications For Unspecified Oab
If your doctor cant find a cause for your OAB, dont worry. Drugs can still help ease your symptoms. Some of these drugs work by relaxing your bladder. They stop involuntary contractions that bring on the urge to urinate. Other drugs help strengthen the tissues around your bladder that may have become weak. The stronger tissue can help improve your bladder control.
When To Seek Medical Help

Any instance of incontinence is reason to seek medical help. It may be a symptom of a more serious condition that needs to be treated.
Even if the underlying cause isnt serious, incontinence can be a major disruption in your life. Its important to get an accurate diagnosis and discuss treatment options with a healthcare professional.
In some cases, incontinence can be a sign of a medical emergency.
You should seek immediate medical attention if you lose control of your bladder and experience any of the following symptoms:
- trouble speaking or walking
Urinary incontinence and treatment for urinary incontinence may result in complications, depending on the cause.
These complications may include:
- Urinary tract infections. UTIs can be caused by wet undergarments against the skin. This may create an environment where bacteria can grow.
- Kidney damage. In some cases where the flow of urine is obstructed, you may experience kidney trouble or kidney failure.
- Cellulitis. This skin infection is caused by bacteria and may cause swelling and pain.
- Medication side effects. Medications used to control urinary incontinence may cause side effects, depending on the medication. Side effects may include dry mouth, nausea, hypertension, or others.
- Catheter side effects. If you have a catheter placed, you may experience side effects such as infection and trauma.
- Mental health side effects. Urinary incontinence may cause feelings of anxiety, depression, or social isolation.
Don’t Miss: Cranberry Juice And Urinary Tract
Will I Have Incontinence For My Entire Life
Sometimes incontinence is a short-term issue that will go away once the cause ends. This is often the case when you have a condition like a urinary tract infection . Once treated, frequent urination and leakage problems caused by a UTI typically end. This is also true for some women who experience bladder control issues during pregnancy. For many, the issues end in the weeks after delivery. However, other causes of incontinence are long-term and related to conditions that are managed throughout your life. If you have a chronic condition like diabetes or multiple sclerosis, you may have incontinence for a long period of time. In those cases, its important to talk to your provider about the best ways to manage your incontinence so that it doesnt interfere with your life.
A note from Cleveland Clinic
It can be embarrassing to talk about bathroom habits with your healthcare provider. This embarrassment shouldnt stop you from treating incontinence, though. Often, your healthcare provider can help figure out the cause of your bladder control issue and help make it better. You dont need to deal with it alone. Talk to your healthcare provider about the best ways to treat incontinence so that you can lead a full and active life without worrying about leakage.
Home Remedies For Urinary Incontinence
Urinary incontinence can be described as the inability to control urination, leading to urine leakage or involuntary loss of urine.
It is a very common, and at times debilitating, urological disorder. According to the National Association for Continence , it affects about 25 million Americans.
Urinary incontinence can be divided into three main types:
- Urge incontinence occurs when an overactive or hyperactive bladder causes a sudden and intense urge to urinate causing involuntary loss of urine
- Stress incontinence occurs when physical activities like vigorous exercise, jumping, coughing, sneezing or even laughing put pressure on the bladder and it releases urine
- Overflow incontinence inability to completely empty the bladder, leading to frequent or constant dribbling of urine
Incontinence can be caused by a number of factors like age , weakened pelvic floor muscles due to surgery or childbirth, enlarged prostate, menopause, an overactive bladder, nerve damage, urinary stones, urinary tract infections and constipation.
Plus, certain foods, drinks and medications may stimulate your bladder and cause temporary incontinence.
It not only can cause discomfort and embarrassment, but can also be harmful if urine is left in the bladder creating a breeding ground for bacteria. Incontinence is not a disease in itself, but a symptom of an underlying condition or disorder.
Here are the top 10 home remedies for urinary incontinence.
You May Like: Signs And Symptoms Of Urinary Incontinence
Incontinence And Alzheimers Disease
People in the later stages of Alzheimers disease often have problems with urinary incontinence. This can be a result of not realizing they need to urinate, forgetting to go to the bathroom, or not being able to find the toilet. To minimize the chance of accidents, the caregiver can:
- Avoid giving drinks like caffeinated coffee, tea, and sodas, which may increase urination. But dont limit water.
- Keep pathways clear and the bathroom clutter-free, with a light on at all times.
- Make sure you provide regular bathroom breaks.
- Supply underwear that is easy to get on and off.
- Use absorbent underclothes for trips away from home.
For more ways to deal with incontinence and other common medical problems in someone with Alzheimers, visit Alzheimers Disease: Common Medical Problems.
How Successful Is Treatment For Urinary Incontinence
The outlook is promising for urinary incontinence treatment. About 80% of people with urinary incontinence can improve or even be cured. The best outcome depends, of course, on getting the correct diagnosis and following your doctors advice to help improve your condition.
American Academy of Family Physicians: Urinary Incontinence: Embarrassing but Treatable.
Jennifer Anger, MD, MPH, urologist, Cedars-Sinai Medical Center, Los Angeles.
Amy Rosenman, MD, co-author, The Incontinence Solution, urogynecologist, Santa Monica, CA, associate clinical professor, UCLA.
National Library of Medicine MedlinePlus Medical Encyclopedia: Urge Incontinence.
Halina Zynczynski, MD, director, division of Urogynecology and Reconstructive Pelvic Surgery, Magee-Womens Hospital, associate professor of obstetrics and gynecology, University of Pittsburgh School of Medicine, Pittsburgh, PA.
American Family Physician: Selecting Medications for the Treatment of Urinary Incontinence.
National Association for Continence: Treatment Options for Incontinence.
American Urological Association: Diagnosis and Treatment of Overactive Bladder in Adults: AUA/SUFU Guideline.
Global Library of Womens Medicine.
Rovner, E. Rev Urol., 2004
Also Check: Over The Counter Urinary Tract Infection Pain Relief
Recommended Reading: Royal Canin Urinary So Canned Food
When Should I See A Doctor About Incontinence
Its important to know that incontinence can be treated. Many people believe that its something that just goes along with aging and is an unavoidable issue. If you find that incontinence is disturbing your daily activities and causing you to miss out on things you typically enjoy, talk to your healthcare provider. There are a wide range of options to treat incontinence.
Different Types Of Incontinence
There are four basic types of incontinence: stress, urge, overflow and functional. They may occur alone, or in combination, especially in seniors.
Stress incontinence is the involuntary leakage of small amounts of urine in response to increased pressure on the bladder . It is present in about 35 per cent of incontinent seniors. It is more common in women, often because childbirth caused the pelvic muscles to relax. It also occurs, usually temporarily, in men who have had prostate surgery.
Urge incontinence is the leakage of large amounts of urine when someone is unable to reach the toilet after getting the urge to urinate. It accounts for 60-70 per cent of incontinence problems in seniors.
Overflow incontinence accounts for 10-15 per cent of urinary incontinence. It occurs when there is an obstruction in the bladder, which causes the bladder to overfill. Often, there is no sensation that the bladder is full. Then, when the bladder contracts, urine is released.
Functional incontinence accounts for 25 per cent of the incontinence seen in institutions. It often happens because a person has difficulty moving from one place to another. Poor vision, hearing or speech may interfere with reaching the toilet or telling caregivers of the need to use the toilet. This type of incontinence can also occur in the home.
Read Also: Urinary Tract Infection When To See A Doctor