Incontinence In The Elderly
Using drugs to manage incontinence in the elderly follows the basic prescribing principle of ‘start low, go slow’. As well as the dose, polypharmacy and coexisting medical comorbidities must be considered.
Antimuscarinics such as oxybutynin and tolterodine are the mainstay for bladder overactivity, but should be used with care. The risk of urinary retention is a concern, as the ageing bladder is often associated with impaired emptying. This necessitates a slow escalation of the dose, frequent review of the response and monitoring of urine output and post-void residual volume.
Newer drugs such as darifenacin and solifenacin are more M3-selective and cross the bloodbrain barrier less readily than non-selective drugs. There is some evidence that non-selective drugs are more likely to cause cognitive dysfunction.14The most recent randomised trial reports that both oxybutynin and solifenacin are well-tolerated in the elderly, but oxybutynin is associated with a reduction in attention compared to placebo.15
What Tests Will Be Done To Diagnose Overactive Bladder
A healthcare provider may order tests to help diagnose overactive bladder. These tests may include:
- Urinalysis. A urinalysis examines the visual, chemical and microscopic aspects of your pee. A provider will look for red blood cells, white blood cells and bacteria. If you have any of them in your pee sample, you may have an infection that causes OAB.
- Urodynamic testing. Urodynamic tests measure how much pee remains in your bladder after you go to the bathroom, how much you pee, how fast you pee and how much pressure is on your bladder as it fills with pee.
- Ultrasound. An ultrasound is a noninvasive imaging test that allows a healthcare provider to take a detailed look at your bladder.
- Computed tomography scan. A CT scan is a noninvasive imaging test that produces 3D images of your bladder.
- Cystoscopy. A healthcare provider will use a special instrument to look inside your bladder from your urethra. The provider typically uses a numbing gel so you dont feel pain in your urethra. In rare cases, they may use general anesthesia, so you arent awake, wont move and wont feel any pain.
Dont Ignore Your Diet
While you may have never thought about it, our bladder and bowel often work in synchronization.
When the bowel is full it starts putting pressure on the empty bladder, making you feel like you need to pee.
So, to steer clear from this situation and prevent an indirect urinary urgency from building up, it is always better to add food items such as green leafy vegetables, fresh fruits, and beans to your diet that keep your bowel relaxed and constipation-free.
Also Check: Urinary Tract Infection When To See A Doctor
How Do I Control Urges When Resetting My Bladder
Controlling your urges is a key step in resetting your bladder. The following strategies may help:
- Stop what youre doing and stay put. Stand quietly or sit down, if possible. Remain as still as possible. When youre still, its easier to control your urges.
- Squeeze your pelvic floor muscles quickly several times . Dont fully relax in between Kegels.
- Relax the rest of your body. Take several deep breaths to help you let go of any tension.
- Concentrate on suppressing your urge to pee.
- Wait until the urge goes away.
- Walk to the bathroom at a normal pace. Dont rush. Continue squeezing your pelvic floor muscles quickly while you walk.
Patience is important. Retraining your bladder usually takes at least six to eight weeks to see results. Talk to a healthcare provider if you have any questions or arent happy with your progress. They may prescribe medications for you to take while youre resetting your bladder to help you achieve the best outcome.
What Are The Complications Of Urge Incontinence
Urge incontinence can affect your mental health. Some people with severe urge incontinence may be afraid to go out in public. They may worry about being too far from a restroom for fear of an accident. These worries may increase your risk of anxiety and depression.
Because urge incontinence causes you to leak a lot of urine, you may want to wear adult diapers or absorbent urinary pads until treatments take effect. Unfortunately, constant exposure to urine can lead to skin rashes and sores.
Read Also: What Causes Urinary Incontinence At Night
Urinary Incontinence In Women: What You Need To Know
-
Urinary incontinence is the accidental loss of urine.
-
Over 25 million adult Americans experience temporary or chronic urinary incontinence.
-
This condition can occur at any age, but it is more common in women over the age of 50.
-
There are four types of urinary incontinence: urgency, stress, functional and overflow incontinence.
-
Behavioral therapies, medications, nerve stimulation and surgery are some of the treatments available for managing urinary incontinence.
What Are Kegel Exercises
Kegel exercises, also called Kegels or pelvic floor muscle training, are exercises for your pelvic floor muscles to help prevent or reduce stress urinary incontinence. Your pelvic floor muscles support your uterus, bladder, small intestine, and rectum.
Four in 10 women improved their symptoms after trying Kegels.9 Kegels can be done daily and may be especially helpful during pregnancy. They can help prevent the weakening of pelvic floor muscles, which often happens during pregnancy and childbirth. Your pelvic floor muscles may also weaken with age and less physical activity.
Some women have urinary symptoms because the pelvic floor muscles are always tightened. In this situation, Kegel exercises will not help your urinary symptoms and may cause more problems. Talk to your doctor or nurse about your urinary symptoms before doing Kegel exercises.
You May Like: Urinary Tract Infection And Dementia
How Is Urinary Urgency And Frequency Treated
Treatment will depend on the type and cause of your urination problems. You may need any of the following:
- Medicines may be given to relax your bladder and decrease urination. You may also need antibiotics if your symptoms are caused by a bacterial infection.
- Sacral nerve stimulation sends electrical signals to your sacral nerve through a small device implanted under your skin. Your sacral nerve controls your bladder, sphincter, and pelvic floor muscles.
- Botox injections into your bladder may help relax your bladder muscle to decrease urgency and frequency.
- Surgery may be done if all other treatments cannot help you control your bladder.
You May Like: Best Way To Get Rid Of Urinary Tract Infection
Signs And Symptoms Of Frequent Urina
If your frequent urination is caused by an overactive bladder , you may or may not display some or all of the aforementioned symptoms.
Serious symptoms may include urinal bleeding, at which point, its advised that you visit a doctor.
If the symptoms are mild, and you just have a frequent urge to go, then there are some great home remedies that you can try to reduce that urge and make your overactive bladder less active.
You May Like: Foods To Help Urinary Tract
Urinary Incontinence In Older Adults
Urinary incontinence means a person leaks urine by accident. While it can happen to anyone, urinary incontinence, also known as overactive bladder, is more common in older people, especially women. Bladder control issues can be embarrassing and cause people to avoid their normal activities. But incontinence can often be stopped or controlled.
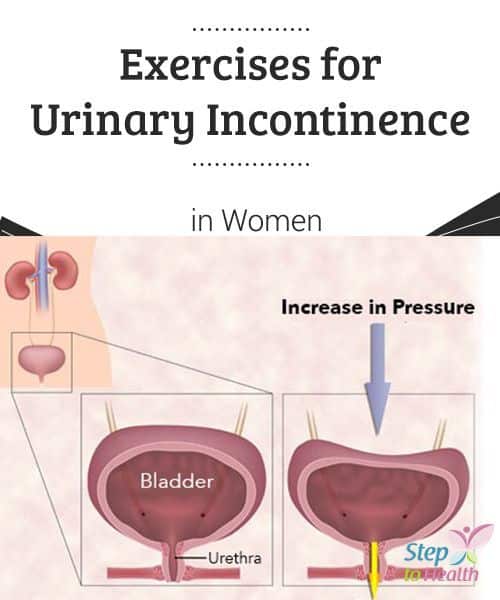
What happens in the body to cause bladder control problems? Located in the lower abdomen, the bladder is a hollow organ that is part of the urinary system, which also includes the kidneys, ureters, and urethra. During urination, muscles in the bladder tighten to move urine into the tube-shaped urethra. At the same time, the muscles around the urethra relax and let the urine pass out of the body. When the muscles in and around the bladder dont work the way they should, urine can leak, resulting in urinary incontinence.
Incontinence can happen for many reasons, including urinary tract infections, vaginal infection or irritation, or constipation. Some medications can cause bladder control problems that last a short time. When incontinence lasts longer, it may be due to:
- Weak bladder or pelvic floor muscles
- Overactive bladder muscles
- Damage to nerves that control the bladder from diseases such as multiple sclerosis, diabetes, or Parkinsons disease
- Diseases such as arthritis that may make it difficult to get to the bathroom in time
Most incontinence in men is related to the prostate gland. Male incontinence may be caused by:
Control Your Urge To Urinate
You may be able to control, or suppress, the strong urge to urinate, which is called urge or urgency suppression. With this type of bladder training, you can worry less about finding a bathroom in a hurry. Some people distract themselves to take their minds off needing to urinate. Other people find that long, relaxing breaths or holding still can help. Doing pelvic floor exercises to strengthen your pelvic floor also can help control the urge to urinate. Quick, strong squeezes of the pelvic floor muscles can help suppress urgency when it occurs, which may help you get to the toilet before you leak.
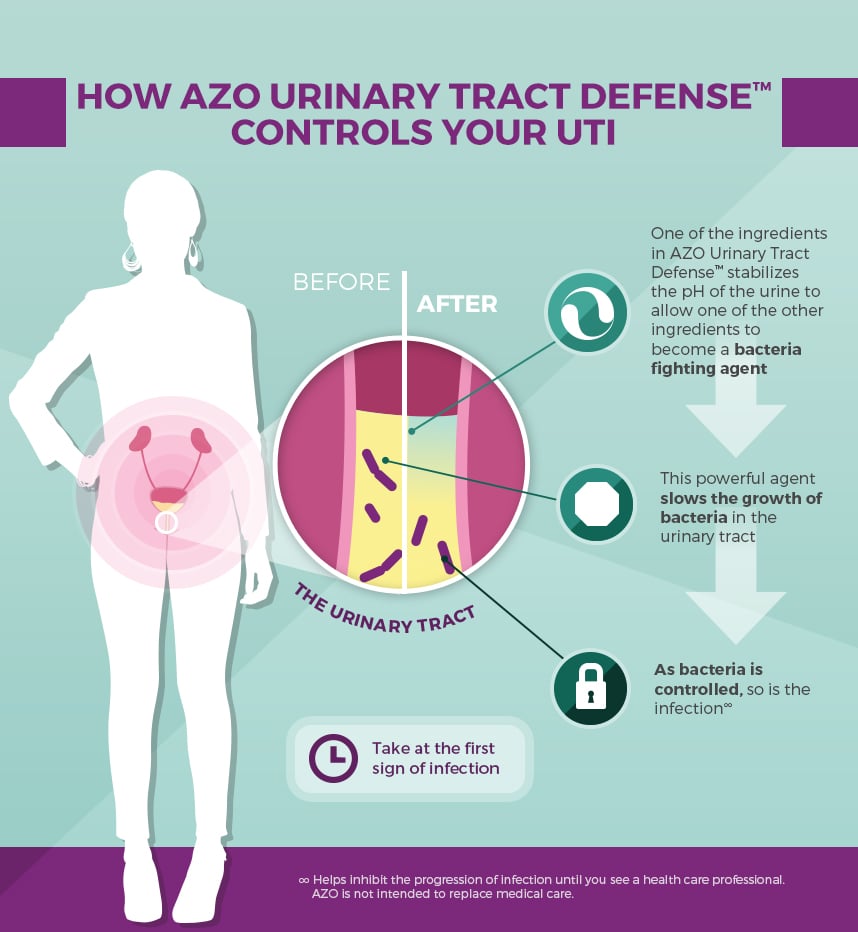
Read Also: Azo Urinary Tract Defense Antibacterial Protection
Behavioral Treatments For Urge Incontinence
One way of dealing with urge incontinence is to simply change some of your behaviors. For instance, if you can anticipate when your bladder is overactive and may be contracting abnormally, you can take action to avoid any mishaps or urine leakage.
Here are some techniques that may be helpful:
- Biofeedback: Biofeedback is a practice that helps you learn how your body normally behaves. When you do, you will know when it is not functioning properly. In the case of urge incontinence, biofeedback can help you recognize when your bladder is overactive.
Two biofeedback techniques are timed voiding and bladder training. To practice timed voiding, you use a chart to record the times that you urinate and when you leak urine. This will give you an idea of your leakage “patterns.” Then you can avoid leaking in the future by going to the bathroom at those times.
With bladder training, you “stretch out” the intervals at which you go to the bathroom. You do this by waiting a little longer before you go. For instance, to start, you can plan to go to the bathroom once an hour. You follow this pattern for a period of time, and then you change the schedule so that you are going to the bathroom every 90 minutes. Then eventually, you lengthen the interval to every two hours, and so on, until you are up to three or four hours between bathroom visits.
Other behavioral tips for preventing urge incontinence include:
What Is The Main Cause Of Overactive Bladder

Conditions or injuries that affect your detrusor muscle cause overactive bladder. Your detrusor muscle is a collection of smooth muscle fibers in the wall of your bladder. These conditions may include:
- Abdominal trauma. Pregnancy and childbirth can stretch and weaken your pelvic muscles. Your pelvic muscles are the muscles and tissues that support the organs in your lower abdomen. Your bladder may sag out of its normal position if your pelvic muscles weaken.
- Nerve damage. Sometimes your body sends signals to your brain and bladder to pee at the wrong time. Certain diseases and trauma can cause nerve damage, including pelvic or back surgery, herniated discs, radiation therapy, Parkinsons disease, multiple sclerosis or a stroke.
- Medications, alcohol and caffeine. All of these can dull your nerves, which affect signals to your brain and cause your bladder to overflow. Diuretics and caffeine may cause your bladder to fill rapidly and potentially leak.
- Infection. An infection, such as a urinary tract infection , can irritate your bladder nerves and cause your bladder to squeeze without warning.
- Extra weight. Having overweight can put extra pressure on your bladder, which can cause urge incontinence.
- Estrogen deficiency after menopause. Hormonal changes may cause urge incontinence. Vaginal-only estrogen therapy can help.
Also Check: Urinary Tract Infection Puppy Treatment
What Questions Should I Ask A Healthcare Provider
- How do you know that I have an overactive bladder?
- Whats the cause of my overactive bladder?
- Whats a normal number of times to pee each day?
- How much should I drink each day?
- What fluids should I drink?
- What fluids should I avoid drinking?
- What foods should I eat?
- What foods should I avoid eating?
- What treatments do you recommend?
- Are there any side effects to your recommended treatment?
- What medications do you recommend?
- Are there any side effects to your recommended medications?
- Are there any other lifestyle changes I can make?
- Can you recommend a support group for people with overactive bladder?
A note from Cleveland Clinic
Overactive bladder is a common condition that causes changes in your bathroom habits, which can be embarrassing. Many people struggle to talk to a healthcare provider about their symptoms. However, providers can help answer any of your questions without judgment. They can determine the cause of your overactive bladder and work with you to develop the best treatment plan. If you have symptoms of overactive bladder, talk to a healthcare provider so you can regain control of your bathroom habits and improve your quality of life.
What Is Urge Incontinence And How Is It Treated
Topics in this Post
There are many different types of urinary incontinence the loss of bladder control. One of the most common types is urge incontinence, which is characterized by a sudden, intense urge to urinate followed by an involuntary loss of urine. You may need to urinate often, including throughout the night.
Urinary incontinence is more common among women with approximately 17% of women and 3% to 11% of men experiencing urge incontinence at some point in their lives. Fortunately, there are many different treatment options for urge continence ranging from conservative to more invasive.
Don’t Miss: What Causes A Man To Have A Urinary Tract Infection
When Should I See A Healthcare Provider
See a healthcare provider if you experience any symptoms of an overactive bladder.
Age-related OAB may develop gradually and slowly worsen over time. If your symptoms develop suddenly and you have heavy leakage, your OAB may be a symptom of another condition, such as an infection or a neurological issue. Its best to have a provider check these symptoms sooner rather than later.
S To Overcoming Overactive Bladder
Overactive Bladder is a common condition often due to ones bladder contracting at any time without warning. This involuntary bladder contraction can give rise to the symptoms of urgency, frequency and urgency incontinence. The key symptom of OAB is urinary urgency , the sudden and compelling desire to urinate that is difficult to postpone. This problem can occur in both women and men, although it is more common in females.
Although OAB symptoms can occur without specific provocation, they may be triggered by exposure to running water, cold or rainy weather, hand-washing, entering the shower, positional changes such as arising from sitting, and getting nearer and nearer to a bathroom, particularly at the time of placing the key in the door to ones home.
12 Steps To Overcoming OAB
The goal of these 12 steps is to re-establish control of the urinary bladder. Providing that the recommendations are diligently adhered to, there can be significant improvement, if not resolution, of OAB symptoms.
You May Like: What Could Cause Urinary Tract Infection
Drop The Triggers For A While
For most of us, urine urgency is not because of a looming disease or condition. Instead, it is typically the excessive intake of certain food and drinks that causes our bladder to fill up quickly and cause urine leakage.
Among these food and drinks items are caffeinated drinks, cold drinks, spicy foods, tomato-rich foods, chocolate, etc.
So, if you decide to cut down on these food items for a while, your urges should reduce.
Pelvic Floor Muscle Training
Your pelvic floor muscles surround the bladder and urethra and control the flow of urine as you pee.
Weak or damaged pelvic floor muscles can cause urinary incontinence, so exercising these muscles is often recommended.
A GP may refer you to a specialist to start a programme of pelvic floor muscle training.
The specialist will assess whether you’re able to squeeze your pelvic floor muscles and by how much.
If you can contract your pelvic floor muscles, you’ll be given an exercise programme based on your assessment.
Your programme should include a minimum of 8 muscle contractions at least 3 times a day and last for at least 3 months. If the exercises are helping after this time, you can keep on doing them.
Research has shown that pelvic floor muscle training can benefit everyone with urinary incontinence.
Find out more about pelvic floor exercises.
Don’t Miss: Can Urinary Tract Infection Cause Dementia
Anticholinergic Drugs For Overactive Bowel
This particular class of medication is used to control the muscle spasms that lead to overactive bladder. Anticholinergic drugs focus on blocking the nerve signals that typically trigger inopportune bladder contractions, reduce the frequency, and the severity of your urge to urinate.
There are several anticholinergic drugs to choose from and they all require a doctors prescription. Most people have very favourable reactions to anticholinergics, though there are a few possible side effects which may include dry mouth, constipation, increased heartbeat and/or drowsiness.
Conservative Ways To Treat Urinary Incontinence Include:
- Dietary changes Try to eliminate or cut back on how much caffeine you consume, such as in coffee and tea. In addition, limit the amount of carbonated drinks and acidic foods, such as oranges and pineapples, in your diet. Caffeine prompts your body to get rid of fluids, which causes you to need to urinate. Also, the acids in carbonated drinks and some foods can irritate your bladder and cause you to go more often.
- Manage constipation For some people, urinary incontinence is a symptom of constipation. Your rectum is located near your bladder and shares many of the same nerves. Hard, compacted stool in your rectum can cause these nerves to be overactive and increase urinary frequency.
- Physical therapy A therapist can explain different exercises to do to strengthen the muscles that help control urination. Also known as Kegels, these exercises are especially effective for stress incontinence but also may help urge incontinence.
Recommended Reading: How Does Copd Affect The Urinary System