Surgical Treatment Options For Men With Sui
Before considering surgery, a full assessment of stress incontinence should be made to determine an individuals suitability for surgery and make a recommendation regarding type of surgery. Such assessment may include:
- Sling surgery with suburethral slings specifically designed for male stress urinary incontinence
- Artificial urinary sphincter
Overall the artificial urinary sphincter is regarded as the gold standard treatment for severe male stress urinary incontinence occurring after radical prostatectomy surgery. Slings, injectable agents and other devices are better suited to men experiencing mild to moderate stress incontinence.
How Does Is Work
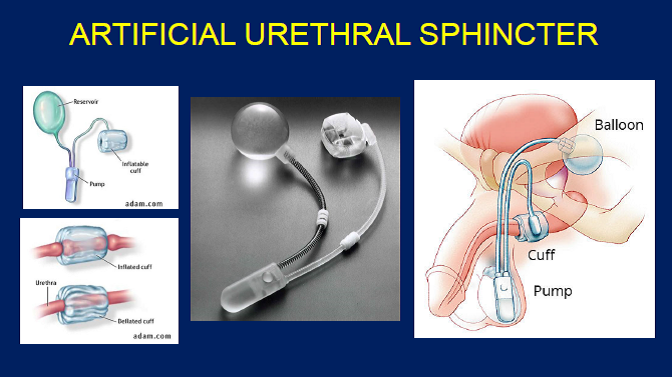
A balloon reservoir that holds fluid sits within the pelvis and keeps a cuff inflated around the urethra, preventing leakage of urine. A pump placed in the labia in women and scrotum in men is then operated to deflate the cuff when you want to empty your bladder. The cuff automatically re-inflates after 3-5 minutes.
Appendix 3 Search Strategy Embase Via Ovid
Last searched in April 2014.
#1. surgery
#37. Bode Brand of Glutaral
#38. Novaruca
#39. Bioglan Brand of Glutaral
#40. Sekumatic
#41. Ecolab Brand of Glutaral
#42. Diswart
#43. Dermatech Brand of Glutaral
#44. Glutarol
#45. Dermal Brand of Glutaral
#46. Cahill May Roberts Brand of Glutaral
#47. ethylenevinyl alcohol copolymer
#48. Enteryx
#90. trisacryl gelatin microspheres
#91. Embosphere Microspheres
#99. low temperature isotropic carbon
#100. LTIC
#134. Colporrhaphia
#135. Bladder neck needle suspension
#136. #1 OR #2 OR #3 OR #4 OR #5 OR #6 OR #7 OR #8 OR #9 OR #10 OR #11 OR #12 OR #13 OR #14 OR #15 OR #16 OR #17 OR #18 OR #19 OR #20 OR #21 OR #22 OR #23 OR #24 OR #25 OR #26 OR #27 OR #28 OR #29 OR #30 OR #31 OR #32 OR #33 OR #34 OR #35 OR #36 OR #37 OR #38 OR #39 OR #40 OR #41 OR #42 OR #43 OR #44 OR #45 OR #46 OR #47 OR #48 OR #49 OR #50 OR #51 OR #52 OR #53 OR #54 OR #55 OR #56 OR #57 OR #58 OR #59 OR #60 OR #61 OR #62 OR #63 OR #64 OR #65 OR #66 OR #67 OR #68 OR #69 OR #70 OR #71 OR #72 OR #73 OR #74 OR #75 OR #76 OR #77 OR #78 OR #79 OR #80 OR #81 OR #82 OR #83 OR #84 OR #85 OR #86 OR #87 OR #88 OR #89 OR #90 OR #91 OR #92 OR #93 OR #94 OR #95 OR #96 OR #97 OR #98 OR #99 OR #100 OR #101 OR #102 OR #103 OR #104 OR #105 OR #106 OR #107 OR #108 OR #109 OR #110 OR #111 OR #112 OR #113 OR #114 OR #115 OR #116 OR #117 OR #118 OR #119 OR #120 OR #121 OR #122 OR #123 OR #124 OR #125 OR #126 OR #127 OR #128 OR #129 OR #130 OR #131 OR #132 OR #133 OR #134 OR #135 OR #136
Don’t Miss: Can Cranberry Juice Cure A Urinary Tract Infection
Urinary Incontinence After Prostatectomy
One side effect of a prostatectomy surgery to remove all or part of the prostate gland is urinary incontinence. In other words, you may leak some urine after the surgery. That can cause embarrassment, discomfort, and other emotional and social problems.
How much urine you leak and for how long can vary. Heres what you need to know about urinary incontinence after prostatectomy.
Overall Completeness And Applicability Of Evidence
Although there are several options for surgical treatment of urinary incontinence postprostatectomy, the search found only one randomised controlled trial comparing AUS implantation and injectable treatment with Macroplastique. For other surgical procedures, such as male sling, ProACT system, other bulking agents and stemcell therapy, the search identified only nonrandomised studies. The three ongoing clinical trials identified in the review update are still in the process of recruiting participants. One study aims to compare ProACT with transobturator sling , and two studies aim to compare the AUS with sling . In future updates of this review, we expect to include the results of these studies.
Therefore, of all the options available for surgical treatment of SUI postprostatectomy there was only limited evidence from one small study of the possible superiority of AUS implantation compared with injection of Macroplastique, especially in men with severe UI, but at a higher cost and risk of complications.
Read Also: Instant Relief For Urinary Tract Infection
What Is An Artificial Urinary Sphincter
Your urinary sphincter is a muscle that controls the urine flow from your bladder. An artificial urinary sphincter is a device that includes:
- a fluid-filled cuff that wraps around your urethra ,
- a pump in your scrotum , and
- a balloon in the abdomen.
The fluid inside the cuff helps keep any urine from leaking out. The cuff will remain closed and filled with fluid until you need to urinate.
Will It Work And For How Long
Following this operation most patients with stress incontinence will be dry or significantly improved. 83% -95% patients are satisfied with the results. About 70% are completely dry, and 90% wear no more than one pad per day. There is a reasonably high risk of requiring further surgery for complications or revision of part of or the entire device at some stage.
Read Also: Cure For Male Urinary Tract Infection
How Does An Artificial Urinary Sphincter Work
The goal of an artificial urinary sphincter is to replace the function of your incompetent natural urinary sphincter. It prevents urine from leaking out unless you want to urinate.
An artificial urinary sphincter is made of 3 parts connected together with plastic flexible tubes:
- A cuff: this goes around your urethra and shuts it tight
- A reservoir balloon: this balloon contains sterile saline and is implanted in your pelvis
- A pump: the pump is implanted in your scrotum and has an activation button that you can palpate and press when you want to urinate
BruceBlaus. Blausen.com staff . “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 . DOI:10.15347/wjm/2014.010. ISSN 2002-4436., CC BY 3.0, via Wikimedia Commons
Are There Any Side Effects
Most procedures have a potential for side effects. You should be reassured that, although all these complications are well recognised, the majority of patients do not suffer any problems after a urological procedure.
Please use the check boxes to tick off individual items when you are happy that they have been discussed to your satisfaction:
You May Like: Foods For Urinary Tract Health
Lifestyle Or Behavioral Changes
If itâs right for your symptoms, your doctor may decide to try changes to your routine and diet first before moving on to medication or surgery.
Bladder training. If you have urgency incontinence , your doctor may tell you to practice holding your urine for a short time when you get the urge instead of going right away. You can start by holding it for 10 minutes. After you successfully do that a few times, you can increase your time. You can also use set times during the day to go, and increase the time in between those regular bathroom trips. You can help your body learn to wait longer by practicing breathing or relaxation techniques. With some effort, you may be able to tame your symptoms and only have to urinate every 3 or 4 hours. Keep in mind that you may not see results right away. But if you stay with it, you should benefit within a few months.
Watching what you eat and drink. Treating your leaks may be as easy as avoiding certain foods and beverages. Cut down on alcohol and caffeine. Many experts believe that these things can irritate the bladder and make urinary incontinence symptoms worse. Cut out coffee, tea, sodas, and alcohol to see if it makes a difference.
Avoiding foods that trigger symptoms. Spicy and acidic foods — like citrus fruits and tomatoes — are common culprits. Others include chocolate and artificial sweeteners. But everyone’s different. You may find food has no effect on you.
Here’s how you do it:
How To Prepare For The Procedure
Before surgery, the doctor will ask for a urine sample. This will be tested to make sure you do not have a urinary tract infection. If you have an infection this should be treated with antibiotics before scheduling the surgery. Your doctor may prescribe antibiotics before, during, and after the operation even if there is no infection, for the sake of preventing any infections.
Your doctor will advise you in detail about how to prepare for the procedure. If you need general anaesthesia you must not eat, drink, or smoke a certain time before surgery. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it several days before surgery. Your doctor will advise you on when you can start taking it again.
Read Also: Homeopet Feline Urinary Tract Infection Supplement 15 Ml
Artificial Urinary Sphincter Surgery
According to the Agency for Health Care Policy and Research, urinary incontinence affects approximately 13 million adults. Men have incontinence rates that are much lower than women, with a range of 1.5â5%, compared to women over 65 with rates of almost 50%. In older men, prostate problems and their treatments are the most common sources of incontinence. Incontinence is a complication in nearly all male patients for the first three to six months after radical prostatectomy. A year after the procedure, most men regain continence. Stress incontinence occurs in 1â5% of men after the standard treatment for severe benign prostatic hyperplasia.
When Is An Aus Recommended
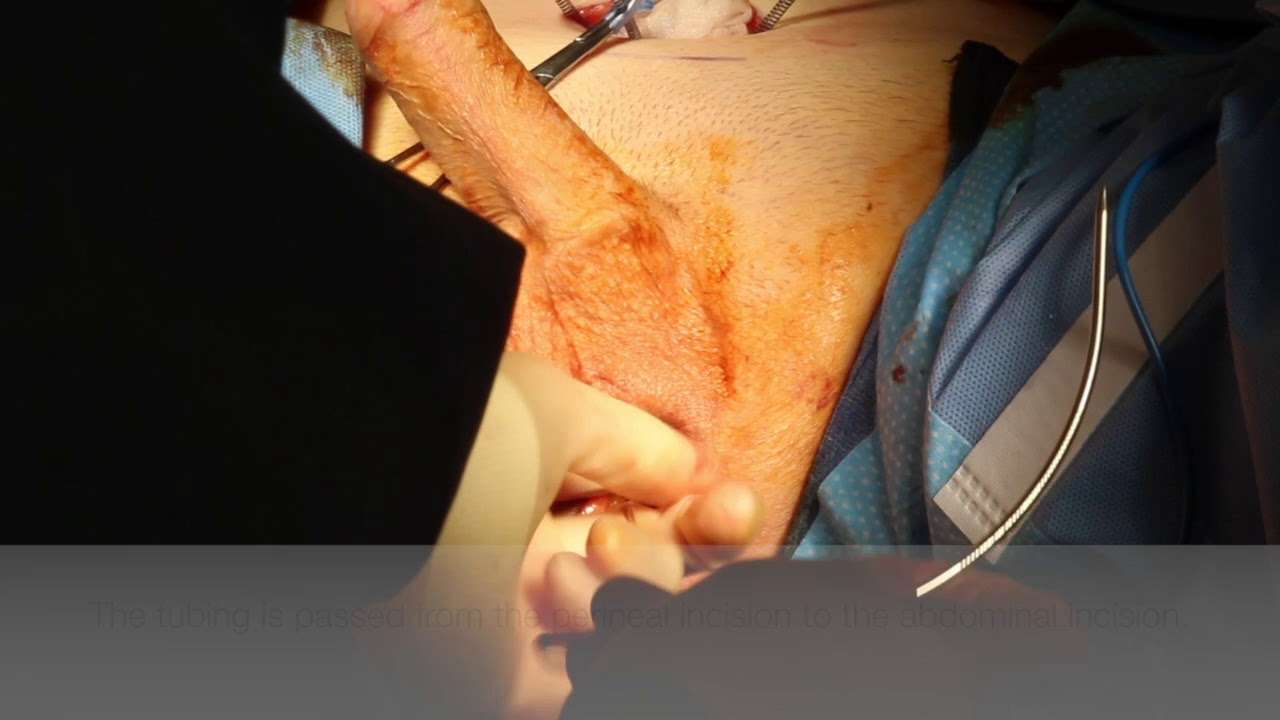
AUS is generally recommended in case of severe urinary incontinence, or if sling implantation has failed to cure or improve your condition. AUS has a long-lasting effect and improves your quality of life.
You should be able to control the pump manually. Before the surgery is scheduled, the doctor or nurse will sit down with you to discuss how the device works and to make sure you feel comfortable using it.
The doctor will do some tests to make sure that there are no contraindications for getting an AUS. As part of this assessment, you may need a work-up including a urodynamic study, a cystoscopy, and a pad test.
Also Check: Urinary Tract Infection Urinating After Sexual Intercourse
What Is The Evidence Base For This Information
This leaflet includes advice from consensus panels, the British Association of Urological Surgeons, the Department of Health and evidence based sources it is, therefore, a reflection of best practice in the UK. It is intended to supplement any advice you may already have been given by your urologist or nurse specialist as well as the surgical team at Addenbrookes. Alternative treatments are outlined below and can be discussed in more detail with your urologist or specialist nurse.
When Will A Doctor Recommend Surgery For Urinary Incontinence
Urinary incontinence is a common problem that doctors see all the time, and they understand youll want to do all you can to help improve it. Discussing your symptoms and how theyre affecting your life is the best way to find the right treatment for you so dont let any feelings of embarrassment hold you back.
But when might your discussion turn to surgery? Your doctor might recommend it if youve tried to manage your condition in other ways such as with lifestyle changes and pelvic floor or bladder exercises (read about urinary incontinence treatment without surgery but these havent helped.
Before surgery is considered, its important you have an accurate diagnosis about the type of urinary incontinence you have . You should also discuss whether you plan to have children if you do, your doctor may suggest delaying surgery.
If youre worried about your symptoms, you can use our Smart Symptom Checker to help you work out what conversation to have with your doctor next.
Also Check: Topical Estrogen For Urinary Incontinence
Artificial Urinary Sphincter Operation
The procedure will be performed in an operating room, either in the hospital or at a surgery center. Your urologic surgeon will insert the device in one of two ways:
- a tiny incision on the upper part of your scrotum or
- two incisions .
This is typically an outpatient procedure but may include an overnight hospital stay. If done as outpatient, you will need to return to the clinic the next day to have your bandages removed.
About Your Urinary Sphincter
Your urinary sphincter is a muscle that controls the flow of urine out of your bladder . When your urinary sphincter is contracted , it blocks the opening of your bladder so urine doesnt leak out.
Figure 1. Urinary sphincter
Normally, your urinary sphincter stays contracted until you choose to relax it to urinate . When you relax your urinary sphincter, urine leaves your bladder and flows through your urethra and out of your body .
Some people have trouble controlling their urinary sphincter. This causes them to leak urine. This can happen after surgery to remove the prostate or radiation therapy to the prostate.
You may need an artificial urinary sphincter if you lose control of your urinary sphincter.
Read Also: Prostate And Urinary Tract Infection
Incontinence Surgery And Recovery After The Incontinence Surgery Procedure
Incontinence, also known as bladder leakage, is a life-altering condition. Surgery to treat incontinence can likewise be life-changing. Before you decide to pursue incontinence surgery for male bladder leakage, youll want to understand the stress incontinence surgical procedures, the incontinence implants available, the SUI surgery recovery process and what it will be like to live with a male sling or artificial urinary sphincter device.
First of all, you should meet with your urologist for a focused physical exam and discussion about treatment goals. Depending on the severity of your incontinence and medical history one or more implantable device may be indicated for your stress incontinence surgery.
Artificial Anal Sphincter Surgery
Fecal incontinence is the inability to control bowel function. The condition can be the result of a difficult childbirth, colorectal disease such as Crohn’s disease, accidents involving neurological injuries, surgical resection for localized cancer, or by other neurological disorders. Severe fecal incontinence may, depending upon the underlying disease, require surgical intervention that can include repair of the anal sphincter, , or replacement of the anal sphincter. Artificial anal sphincter is a very easy-to-use device implanted under the skin that mimics the function of the anal sphincter.
Recommended Reading: Apple Cider Vinegar For Urinary Tract Infection
Hair Removal Before An Operation
For most operations, you do not need to have the hair around the site of the operation removed. However, sometimes the healthcare team may need to remove hair to allow them to see or reach your skin. If the healthcare team consider it is important to remove the hair, they will do this by using an electric hair clipper, with a single-use disposable head, on the day of the surgery. Please do not shave the hair yourself, or use a razor for hair removal, as this can increase the risk of infection to the site of the operation. If you have any questions, please ask the healthcare team who will be happy to discuss this with you.
Things To Keep In Mind
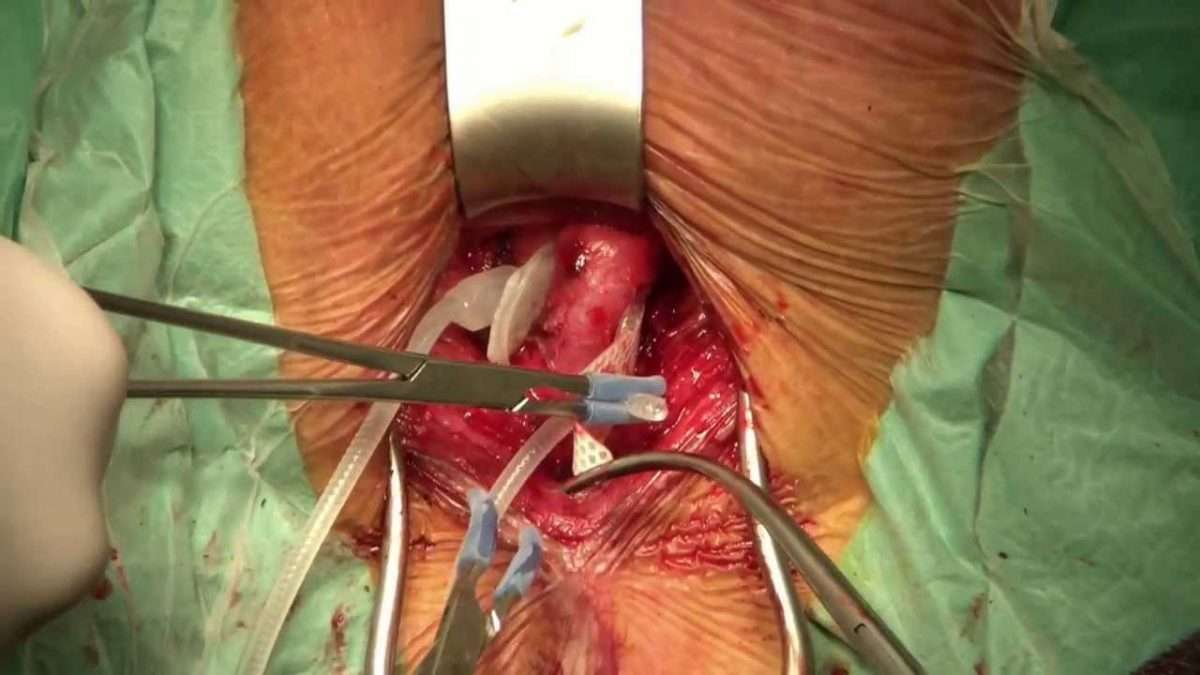
It’s important to tell your other health care providers that you have an artificial urinary sphincter. Implants are safe for getting an MRI, if needed. However, if youre having a dental procedure, youll likely need additional antibiotics. Or if you need a urinary catheter, a urologist or experienced physician will need to deactivate the cuff to prevent any damage.
You May Like: Canine Urinary Tract Infection Home Remedies
What Kind Of Surgery Is Effective For Female Urinary Incontinence
If you have stress incontinence, the 3 surgical options are usually colposuspension, sling surgery and vaginal mesh surgery. All 3 are known to effectively treat some women. But they dont help everyone, and its not possible to say for certain whether a particular surgery will be better for you.
Some women also get problems called complications after these types of surgery. These can include problems emptying your bladder fully, needing to pee urgently, or damage to your bladder or bowel. Generally, studies show that about 1 to 10 in 100 women get these problems .
In most cases, it isnt possible to say if 1 type of surgery is more likely to cause complications. For example, research suggests that pelvic organ prolapse may be more common after colposuspension than mesh surgery, with up to 25 women in 100 getting this at some point after colposuspension . But other complications can happen after mesh surgery and in fact its not recommended on the NHS at the moment because of these .
If you have urge incontinence, surgery is less likely to be effective, and procedures such as nerve stimulation or botox injections are more commonly recommended . Surgery is usually only considered in rare cases, if other treatments havent worked.
Why It Is Important To Do This Review
Urinary incontinence after prostate surgical procedures is one of the most feared problems by men and urologists because it can have a major negative impact on morale and QoL. The surgical options use different types of prosthesis such as AUS, male slings, and injectable substances, but many of them are very expensive and invasive. Although the literature has several studies on this subject, the quality of the published evidence on efficacy, safety, complications, and longterm results is unknown. There are few comparative studies and only two narrative reviews. Therefore, the purpose of this systematic review is to summarise the evidence available from randomised controlled trials to identify which interventions are effective and cost effective, and thus to enable men with urinary incontinence after prostate surgery and their care providers to decide on the best management.
Recommended Reading: Causes Of Urinary Incontinence In Elderly Males