Increased Risk Of Overactive Bladder In Patients With Idiopathic Parkinsons Disease: Insight From A Nationwide Population
-
Roles Conceptualization, Investigation, Methodology, Writing original draft
Affiliation Department of Neurology, China Medical University Hospital, China Medical University School of Medicine, Taichung, Taiwan
-
Affiliation Department of Neurology, China Medical University Hospital, China Medical University School of Medicine, Taichung, Taiwan
You May Like: Pfnca Wellness Programs
Diagnosis Of Constipation In Parkinsons Disease
Diagnosis of constipation may include:
- medical history
- detailed description of symptoms
- physical examination.
Medical problems other than Parkinsons disease can also cause constipation. Your doctor may wish to do tests to rule out other possible causes. The tests depend on the medical condition under investigation.
What Are They Wearing
Although you should allow someone with Parkinsons Disease to assert their individuality, you can ensure they are not wearing awkward clothing. Unnecessary zips and buttons on clothing can make it difficult to remove clothing in time, resulting in leakages. Try and encourage them to wear simple clothing that is fast and efficient to remove.
Read Also: Fruits Good For Urinary Tract
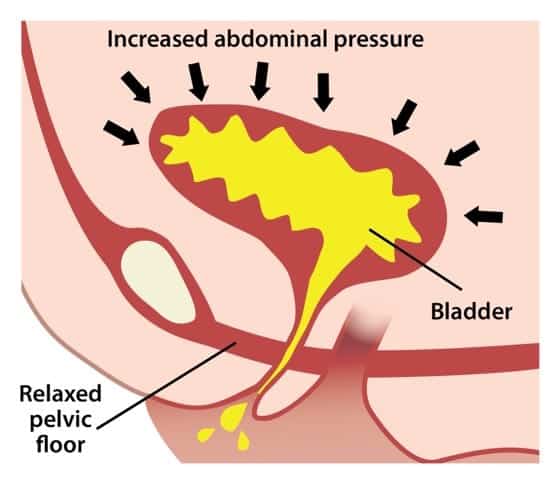
What Happens To Someone Who Has Urinary Incontinence
The pelvic floor consists of a hammock of muscles, ligaments, and connective tissue, which covers the bottom of the pelvic cavity and assists in supporting the abdominal and pelvic organs. The pelvic floor maintains continence of bowel and bladder and plays an important role in sexual function.
The pelvic floor muscle consists of three layers and has fast and slow-twitch fibers to assist with support and sphincter properties. The muscle is the same in women and men and both sexes benefit from maintaining good strength and tone of the pelvic floor muscle.
As we age and with certain diseases such as PD our muscles become weak and the signals do not always tell the muscles to tighten up when they need too. Add a few pounds to the belly region also and you have the perfect storm for Peezing, Peelaughing, as well as a host of other words for embarrassing moments due to urinary incontinence or urgency!
Read Also: Diseases Similar To Parkinsons
The Pathophysiology Of Voiding Dysfunction In Parkinsons Disease

The hypothesis most widely accepted is that in healthy individuals basal ganglia output has an overall inhibitory effect on the micturition reflex.In PD animal modelsdepletion of dopaminergic neurones induces overactive bladder, and D1 receptor agonists produce inhibition of the micturition reflex in a dose-dependent manner while D2 receptor stimulation facilitates micturition. In PD degeneration of dopaminergic neurons in the substantia nigra leads to detrusor hyperactivity, through an inability to activate the D1-mediated tonic inhibition. A parallel mechanism may be that in PD, the inhibitory dopaminergic neurons originating in the substantia nigra may be more damaged than the excitatorydopaminergic neurons originating in the VTA, thereby inducing urgency and frequency.
Don’t Miss: The O Shot For Urinary Incontinence
Ui And Adverse Health Outcomes
The mean follow-up of time of the participants was nearly 8 years . We employed a Cox proportional hazards model adjusted for age, sex, and education to examine the association of baseline UI with incident parkinsonism. Baseline UI was associated with incident parkinsonism . Since we treated UI as a numerical scale, inspection of the hazard ratio suggests that an individual with severe incontinence , had about a 30% increased risk of developing parkinsonism as compared to an individual without incontinence.
Since the pathologic basis for parkinsonism in older adults with and without a clinical diagnosis of PD may vary , we repeated this analysis excluding 65 cases with a clinical diagnosis of PD. Baseline UI remained associated with incident parkinsonism . In a final model, adding terms for seven chronic health conditions and BMI did not attenuate the association of UI with incident parkinsonism .
In further analyses, we examined whether baseline UI was associated with other adverse health outcomes. Baseline UI was also associated with risk of death and incident ADL and mobility disability, but was not associated with incident MCI or AD dementia . These findings were unchanged when we controlled for seven chronic health conditions and BMI .
The Cross-Sectional and Longitudinal Associations of Baseline Urinary Incontinence and Global Cognition in Community-Dwelling Older Adults*
| Model Terms . |
|---|
Prevalence Of Luts In Pd
The pooled prevalence of LUTS was 61% .
Figure 2. Forest plot showing the prevalence of LUTS , urinary incontinence , urinary retention , and post-void residual volume 100 ml in PD patients.
Figure 3. Frequency of LUTS or its subtypes in PD patients. The x-axis shows different kinds of LUTS while the y-axis shows the percentage.
For subgroup analyses, we found that H& Y stage, gender, and different diagnostic tools may be cause of heterogeneity related to the prevalence of LUTS . The pooled prevalence of LUTS was 59% in PD with H& Y stage < 3, whereas 70% in PD with H& Y stage 3. The pooled prevalence of LUTS was 62% in male PD patients, whereas 54% in female PD patients.
Table 2. Prevalence of LUTS or subtypes: results of the subgroup analysis.
No significant publication bias was found by Begg’s funnel plot .
Don’t Miss: Self Care For Urinary Tract Infection
Tips For Caregivers: Management
Medications are available to calm an overactive bladder, if overactive bladder is the cause of the incontinence. But some have side effects that can make dementia worse. Talk with the doctor about options that apply to the person youre caring for. In some cases, where incontinence is caused by an underlying medical condition, treating the condition may help.
How You Can Tackle Your Loved Ones Incontinence
While it will be difficult to know when your loved one might experience urine leakage, the two of you will feel calmer and more relaxed if youre prepared.
Weve already talked about making a clearer path to the toilet but what else can you do? Well, picking loose fit clothing with an elasticated waistband that can be quickly removed will be another help for those with Parkinsons when theyre trying to undress quickly in front of the toilet. This should also help them to feel more comfortable when moving about.
Whether your loved one needs a little assistance or a lot of assistance, check out these guides for more incontinence care tips.
And of course, TENA products including pants, pads and incontinence bed sheets will give your loved one the best protection, so both of you can be reassured and confident no matter when a leak happens.
Read Also: How Does A Male Get Urinary Tract Infection
Whats Next For Those Suffering From Urinary Incontinence
I decided I did not want to add another medication to the medicine bag. I was trying to see if there was something I could do besides resigning myself to wearing pads or some other incontinence protection all the time. At 53 years old, I wanted to see if there was a way I could help myself.
Part 2 of this article will address my experiences. I plan to discuss what I lovingly refer to as PEE PEE PT physical therapy to help treat urinary incontinence.
Recommended Reading: On And Off Phenomenon
Luts Estimated To Be Up To 65% In Patients With Pd
The reported prevalence of LUTS in patients with PD ranges from 38% to 71%.- However, it has been difficult to determine to what extent PD contributes to LUTS. Men older than 60âyears-of-age might have bladder outlet obstruction as a result of prostate hyperplasia. Women might have stress urinary incontinence. âIdiopathic DOâ can occur in men and women aged older than 65âyears due in part to latent brain ischemia. Some of the studies were published before the diagnosis of MSA was recognized. In recent studies of PD patients who were diagnosed according to modern criteria,, the prevalence of LUTS was found to be 27â63.9% using validated questionnaires,- or 53% in men and 63% in women using a non-validated questionnaire that includes a urinary incontinence category, with all of these values being significantly higher than the incidence rates in healthy controls. The majority of patients had onset of bladder dysfunction after appearance of motor disorder. Correlations have been shown between bladder dysfunction in patients with PD and neurological disability, and bladder dysfunction and stage of disease, both suggesting a relationship between dopaminergic degeneration and LUTS. However, Campos-Sousa etâal. did not find such a correlation.
You May Like: New Device For Female Urinary Incontinence
Assignment Of Interventions: Allocation
Sequence generation
Participants who provide written informed consent will be randomised using a computer generated system to either TTNS intervention or non-active stimulation arm and will be minimised on two factors: severity of urinary symptoms, as reported at study baseline by the IPSS in the Clinical Assessment Form, that is, mild, moderate or severe and status on antimuscarinic medication, that is, treatment naïve, failed or continuing such treatment.
Concealment mechanism
A web-based randomisation system will be used.
Implementation
Implementation will be by staff at the Centre for Healthcare Randomised Controlled trials Clinical Trials Unit at Aberdeen.
Strategies For Managing Nocturia In Pd
Despite the high prevalence of nocturia and impact on QoL, treatment options for managing this problem are currently limited and are often poorly tolerated or ineffective in PD. Guidance on nocturia treatment is limited, and most treatment options are derived from guidance around general management of urinary symptoms in neurological patients., ,
You May Like: Azo Urinary Tract Defense Vs Azo Urinary Pain Relief
Other Treatment Options To Strengthen The Pelvic Floor
There may be some alternative treatments available as well, including:
All of these have the potential to assist with bladder/urgency issues.
The goal of this article was to open up a dialogue about incontinence and urgency and Parkinsons disease. It is one of those embarrassing non-motor issues that many of us, regardless of our age, have as a result of being diagnosed with Parkinsonâs.
The good news is that there are things that can be done to help that do not necessarily include medication! Exercise, diet, therapy, and a willingness to open up about this common issue with those of us with Parkinsons disease is very important. We need to keep talking about it!
Nocturnal Sleep Disturbances And Nocturia
Nocturnal disturbances can be observed in 70% of patients with PD and include PD-related motor symptoms occurring at night PD treatment-related disturbances psychiatric symptoms and other sleep disorders, including insomnia, rapid eye movement behavioral disorder , RLS, and periodic leg movements . The urge to urinate is an important reason for awakening at night and is a potentially amenable cause for sleep disturbances in PD. However, patients whose sleep is disturbed because of other reasons may void because they are awake, not necessarily because of the urge to urinate. Known as convenience void, these voids are not therefore reflective of bladder pathology.
Recommended Reading: Urinary Tract Test At Home
Way Of Producing Adult Nerve Cells Aids Memory Eases Anxiety In Mice
In a 2019 article for the University of Michigans health blog, author Jane Racey Gleeson noted that For PD patients, bladder issues are often due to fluctuations in dopamine levels affecting the bladder muscles and nerves, which are critical to how it functions. PD is also thought to impact the nerve pathway between the bladder and the area of the brain that controls bladder function.
My sister says that her bladder medication helps with her urgency issues most of the time, but not always. She wears incontinence pads, especially at nighttime.
All of this is so embarrassing, Bev said. I never thought this would be such a problem for me.
In addition to medication, other treatments for bladder control include deep brain stimulation and kegel exercises, which help strengthen the pelvic floor muscles that surround the bladder. Implants and percutaneous tibial nerve stimulation are also options.
Managing bladder problems can pose additional challenges for people with PD. Complicating the urgency issue are Bevs mobility problems. She cant always move quickly enough to get to the bathroom in time. I know that this is very frustrating for her.
Although this was a sensitive topic to write about, both Bev and I wanted others who may be experiencing the same issues to know theyre not alone.
You May Like: Signs Of Dehydration In Elderly With Dementia
Increasing Your Fibre Intake
Eating the right amount of fibre and drinking enough fluids can help if you have constipation.
To get more fibre in your diet:
- choose a breakfast cereal containing wheat, wheat bran or oats, such as Weetabix, porridge or bran flakes.
- eat more vegetables, especially peas, beans and lentils.
- eat more fruit fresh, stewed, tinned or dried. High fibre fruits include prunes or oranges.
- drink plenty of fluids throughout the day to avoid dehydration. Lots of fluids are suitable, including water, fruit juice,
- milk, tea and squashes. Cut out caffeine to avoid overstimulation of your bladder.
If you find it difficult chewing high-fibre food, you can get some types which dissolve in water. You can also get drinks which are high in fibre.
Try to increase how much fibre you get gradually to avoid bloating or flatulence .
A dietitian can give you further advice. Ask your GP, specialist or Parkinsons nurse for a referral.
Also Check: On Off Phenomenon
Don’t Miss: Garden Of Life Dr Formulated Probiotics Urinary Tract+
Livdry Incontinence Productsdelivered Discreetly With Free Shipping
As you navigate new and progressing symptoms,it can seem overwhelming. TYE Medical offers an easy way to evaluate, compare,and purchase the incontinence supplies you need.
You can shop our online store to compare products andtake advantage of our Product Finder Tool to help make apersonalized choice. If you have questions, our friendly customer service teamis standing by to help.
You can also take advantage of discreet, free shipping on all orders!
Storage Symptoms In Pd
The pooled prevalence of storage symptoms was 59%. Polyuria was the most prevalent type of LUTS in the patients with PD followed by OAB , nocturia , frequency , urgency , and incontinence . The results were almost the same with those reported previously . OAB was the second most prevalent storage symptom. It was urinary urgency, usually accompanied by increased daytime frequency and/or nocturia, with urinary incontinence or without according to the International Continence Society report .
Storage symptoms were frequent in PD because degeneration of dopaminergic neurons might lead to urination irritative symptoms in PD . Striatum functionally controlled the urine storage. Disruption of D1-GABAergic direct striatal output pathway may cause bladder hyperactivity in PD which had been validated in SPECT and animal studies . Besides, objective assessment with urodynamics showed that detrusor overactivity occur in 4593% of PD patients, which was the most prevalent cause to OAB in PD .
We found that the prevalence of urinary incontinence was 31% in the male PD patients, whereas 43% in female patients with PD. These results suggest that both age and gender influence the outcome of estimated prevalence.
The majority of studies were rated as low quality because of small sample sizes and other reason, although the results were robust in sensitivity analysis. Accounting for aforementioned factors, the prevalence results of urinary incontinence should be interpreted with caution.
Recommended Reading: Can Vitamin D Cause Urinary Tract Infections
What Kind Of Incontinence Does Parkinsons Disease Cause
Incontinence is considered a non-motor symptom of Parkinsons Disease, which is mainly considered to be a movement disorder. This means that much more research and emphasis has gone into the more noticeable motor issues that define the disease and not the prominent non-motor problems that accompany the disease.
This also means that the medication prescribed already to control a persons motor functions doesnt necessarily have any effect on non-motor-related symptoms, such as incontinence, which need to be addressed separately and discussed with your doctor. Identifying and treating incontinence issues arent just about increasing personal comfort. Its about dignity. Its about confidence. Its about quality care.
Bladder And Constipation Problems
Parkinsons commonly leads to problems with constipation and bladder control, including urinary urgency, frequency, retention and nocturia.
These problems add to the challenge of living with Parkinsons and can have a negative effect on a persons quality of life. It is important to seek help in managing these problems, as both issues can be effectively managed.
Read Also: Long Term Prognosis Of Parkinsons Disease
Read Also: Do Probiotics Help With Urinary Tract Infections
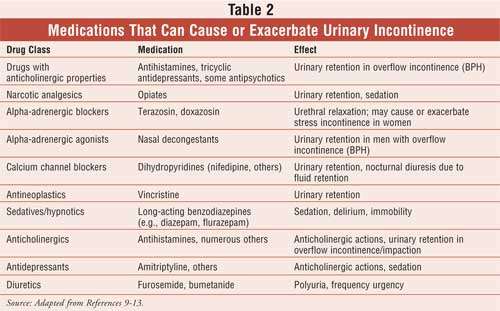
What Medications Help To Treat Urinary Incontinence
So back to the TV ads for urinary incontinence that have us adding MORE medication to our already full medication bag here are many medications that can help this problem. Medications include:
- Phenoperidine fumarate
Do we really want to add that medication to the already growing list to our medications? The answer is YES!
Urinary Incontinence In Parkinsons Disease
The most common urinary difficulty experienced by people with PD is a frequent and urgent need to urinate. This may occur even when the bladder is not full. Recent research studies estimate approximately 27-39% of people with PD experience urinary difficulties, although urinary incontinence only develops in about 15% of those with PD. Bladder issues are more common in the later stages of PD.2
Recommended Reading: Best Treatment For Urinary Retention
Urinary Tract Infection In Parkinsons Disease
Article type: Review Article
Authors: Hogg, Elliota | Frank, Samuela | Oft, Jillianb | Benway, Brianc | Rashid, Mohammad Haruna | Lahiri, Shourid*
Affiliations: Department of Neurology, Cedars-Sinai Medical Center, Los Angeles, CA, USA | Department of Infectious Diseases, Cedars-Sinai Medical Center, Los Angeles, CA, USA | Department of Urology, Cedars-Sinai Medical Center, Los Angeles, CA, USA | Departments of Neurology, Neurosurgery, and Biomedical Sciences, Cedars-Sinai Medical Center, Los Angeles, CA, USA
Correspondence: Correspondence to: Shouri Lahiri, MD, Departments of Neurology, Neurosurgery, and Biomedical Sciences, Cedars-Sinai Medical Center, 8700 Beverly Blvd., Los Angeles, CA 90048, USA. E-mail: .
Keywords: Parkinsons disease, urinary tract infection, delirium, falls, exacerbation
DOI: 10.3233/JPD-213103
Journal: Journal of Parkinsons Disease, vol. Pre-press, no. Pre-press, pp. 1-15, 2022
Abstract
Recommended Reading: Azithromycin Urinary Tract Infection Dose