What Are Some Of The Different Types Of Urinary Incontinence
The following are some of the different types of urinary incontinence:
-
Urgency incontinence: This is the inability to hold urine long enough to reach a restroom. It can be associated with having to urinate often and feeling a strong, sudden urge to urinate. It can be a separate condition, but it may also be an indication of other diseases or conditions that would also warrant medical attention.
-
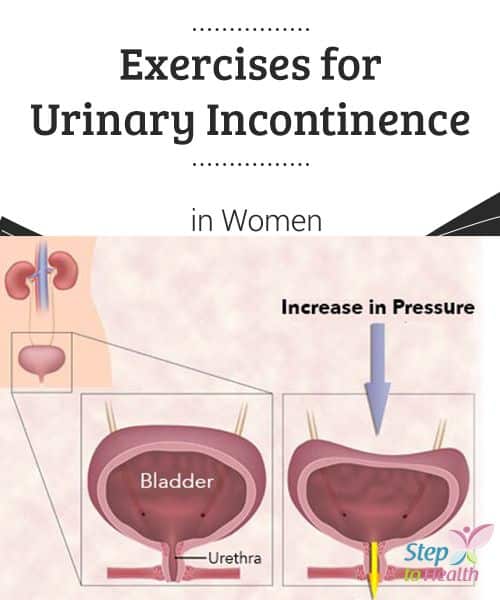
Stress incontinence: This is the leakage of urine during exercise, coughing, sneezing, laughing, lifting heavy objects or performing other body movements that put pressure on the bladder.
-
Functional incontinence: This is urine leakage due to a difficulty reaching a restroom in time because of physical conditions, such as arthritis, injury or other disabilities.
-
Overflow incontinence. Leakage occurs when the quantity of urine produced exceeds the bladders capacity to hold it.
Why Am I Leaking Urine All Of A Sudden
Incontinence can happen when the bladder muscles suddenly tighten and the sphincter muscles are not strong enough to pinch the urethra shut. This causes a sudden, strong urge to urinate that you may not be able to control. Pressure caused by laughing, sneezing, or exercising can cause you to leak urine.
Female Bladder Leakage: Solutions To Get Control | Christopher Tarnay, Md | Uclamdchat
How Is Leaking Urine Diagnosed
Your doctor will have to determine the type of urinary incontinence you have.
Starting a few days ahead of your appointment, your doctor might ask you to keep a bladder diary, MedlinePlus says. The diary would track how much and when you drink liquids, when and how much you urinate, and whether you leak urine.
During the appointment, your doctor will ask about your medical history and symptoms and perform a physical exam. This might include a rectal exam and, for women, a pelvic exam. They might also have you cough or do some other simple maneuver that can initiate the leaking.
To make a diagnosis, your doctor might also run some tests, including:
- Urine and/or blood tests
Don’t Miss: Science Diet Urinary Hairball Control
What Makes Yale Medicine’s Approach To Treating Female Incontinence Unique
Incontinence is a difficult subject for patients to talk about. Here at Yale Medicine, we know the best conversations start with listening. We guide you towards treatments that best match your goals and lifestyle.
We are experts in the latest non-surgical and surgical techniques, and we have an established Urogynecology fellowship program. “We are training the future urogynecologists and that makes us stay sharp,” Dr. Harmanli says. “Plus, at Yale, we are surrounded by other specialists such as urologists, gynecologists, and colorectal surgeons with whom we can coordinate your care.”
At Yale Medicine Urogynecology & Reconstructive Pelvic Surgery, you will work with not only doctors but physical therapists and our nurse practitioner Cherrilyn Richmond, who will coach you through pelvic floor exercises.
Furthermore, Yale researchers are at the forefront of developing new innovative treatment modalities that in 20 years, Dr. Harmanli trusts, ” going to fix most these problems.”
Related Conditions And Causes Of Urinary Incontinence
Fecal incontinence is light to moderate bowel leakage due to diarrhea, constipation, or muscle or nerve damage.
As described in the section above on causes of urinary incontinence, common conditions may contribute to chronic urinary incontinence, including: urinary tract infection , constipation, interstitial cystitis or other bladder conditions, nerve damage that affects bladder control, side effects from a prior surgery, and neurological disorders.
Recommended Reading: Urinary Tract Health For Dogs
Nonsurgical Treatment Options For Ui
Fortunately, there are several nonsurgical treatments for urinary incontinence. From training your bladder and pelvic floor exercises to using a urethral support device, there are different options you can try to manage your symptoms. We recommend discussing your options with a doctor before deciding on the best course of action.
In some cases, your doctor might recommend lifestyle changes to help manage and prevent the symptoms of urinary incontinence. These range from adjustments to your diet, to exercise habits to management techniques between bathroom breaks. Common nonsurgical treatments for urinary incontinence are:
Why Am I Leaking Urine All Of A Sudden What Causes Female Urinary Incontinence Can Uti Cause Urine Leakage
Sudden onset of incontinence, or urine leakage, should always warrant a trip to the doctor. There are several different causes of urine leakage and itâs important to identify prior to any treatment being initiated. The more common types of incontinence in women are stress urinary incontinence and urgency urinary incontinence.
Stress urinary incontinence is caused by a weakness in the sphincter muscle of the urethra , a highly mobile urethra, or both. A highly mobile urethra is seen when the pelvic floor tissues are weak and relaxed. Women will experience leakage of urine with activity, such as coughing, laughing, sneezing, and exercising. The most common risk factor for stress urinary incontinence is having a history of a vaginal childbirth, but it can occur in anyone due to other factors such as muscle strength and activity level. For example, women who do very heavy weightlifting may experience stress urinary incontinence while lifting heavy weights, but if they never did such activities, they might not experience incontinence.
Many people have mixed incontinence, with symptoms of both stress urinary incontinence and urgency urinary incontinence causing urine leakage. In this situation the urologist would typically address the type of incontinence that is most impacting your quality of life first, as the treatments are quite different.
Also Check: Can Clarithromycin Be Used To Treat A Urinary Tract Infection
What Are The Symptoms Of Bladder Control Problems
Signs and symptoms of urinary incontinence can include
- leaking urine during everyday activities, such as lifting, bending, coughing, or exercising
- being unable to hold in urine after feeling a sudden, strong urge to urinate
- leaking urine without any warning or urge
- being unable to reach a toilet in time
- wetting your bed during sleep
- leaking during sexual activity
Amping Up Your Treatment: Medications And Surgery
When more conservative measures have failed, medications – then surgery – are the alternatives, says Galloway.
Medications: No drug helps with stress incontinence, but a class called anticholinergics does help with urge incontinence.
These drugs include Detrol, Oxytrol, Ditropan, and Sanctura — all with similar effectiveness and similar side effects, like dry mouth and constipation, says Galloway.
Medications like Enablexand Vesicare are more effective in controlling the bladder, but don’t cause constipation, he adds.
A transdermal patch called Oxytrol has also been effective, says Galloway, who adds that skin irritation at the patch site does occur in some patients.
Surgery: There are 300 surgical options to treat incontinence, says Brubaker.
“The hard part is picking the surgery that has the best chance of working well for that woman long-term,” he says. “Surgery can create problems. It can cause difficulty in urinating, worsen an urge incontinence problem, or it can do nothing to solve the problem.”
“It helps the urethral sphincter remain closed when abdominal pressure tries to open it. At least, we think that’s how it works,” he says. “We have only five-year outcomes on one group of these devices. But they look promising.”
“Before having any surgery, ask your doctor for names of other patients who have had the procedure in question,” says Galloway.
“Talk to them, find out how it worked. You’ll be in a much better position to decide what to do.”
Show Sources
Read Also: Royal Canin Urinary Wet Food
Bladder Structure And Function
The bladder, urethra and urinary sphincters work in concert to store urine at low pressure and to void voluntarily at socially convenient or appropriate times. The detrusor muscle and internal urethral sphincter are predominantly smooth muscle, whereas the external urethral sphincter and pelvic floor muscles are predominantly striated muscle. The bladder lumen is lined with epithelial cells and the basement membrane that protect the underlying detrusor muscle from toxins contained in the urine and enable communication with neural cells that coordinate storage and voiding phases .
Anatomy and histology of the female bladder
The sympathetic nervous system predominates during the storage phase and maintains continence through the paravertebral ganglia, the hypogastric nerves and hypogastric plexus. The parasympathetic system coordinates the voiding phase, through the sacral plexus and pelvic nerves 39. Afferent signals from the urothelium and bladder wall are transmitted through to the thalamus the balance between storage and voiding is maintained by the central pontine micturition centre . The neurotransmitters responsible for execution of these commands are acetylcholine and noradrenaline.
Neurological control of the urinary bladder
Forms Of Urinary Incontinence That Affect Men Only
- Benign prostatic hyperplasia affects about 50 percent of men over the age of 60, and 90 percent over the age of 85 an enlarged prostate can cause sudden and frequent urges to urinate.
- Peyronies disease is the result of injury or damage to penile tissue, causing an abnormal curvature.
- Painful inflammation of the prostate gland
You May Like: Yeast Vs Urinary Tract Infection
What Your Treatment Will Involve
Your healthcare professionals recommended treatment plan will depend on the cause of your incontinence. An underlying medical condition may require medication, surgery, or other treatments.
In certain situations, they may not be able to cure your bladder incontinence. In these cases, they will likely provide steps you can take to manage your condition.
Treatment options for urinary incontinence may include:
You cant prevent all cases of urinary incontinence, but there are steps you can take to reduce your risk of developing it.
For example, try to:
What To Do If You Are Leaking Urine

– Do daily pelvic floor exercises. Pelvic floor exercises can be effective at reducing leaks, but it’s important to do them properly. … – Stop smoking. … – Do the right exercises. … – Avoid lifting. … – Lose excess weight. … – Treat constipation promptly. … – Cut down on caffeine. … – Cut down on alcohol.
Read Also: What Are The Symptoms Of Urinary Tract Infection In Males
Bladder And Bowel Dysfunction
Patients often complain of urinary urgency, frequency, hesitancy, and incontinence. Incontinence can occur in the setting of a tonically contracted bladder that is incapable of filling completely or with a denervated distended bladder that overflows. It is often not possible to determine the nature of bladder dysfunction by history. Measurement of the volume of postvoiding residual urine, either by catheterization, by ultrasound, or by urodynamic studies, is essential for distinguishing between a spastic and denervated bladder. Bladder dyssynergia, an impairment of sphincter and detrusor coordination, is also a cause of hesitancy and incomplete voiding. Patients with urinary retention are susceptible to urinary tract infections, and such infections may trigger MS relapses by stimulating the immune system.
Bowel dysfunction is common in MS and is presumably caused by spinal cord plaques. Chronic constipation can worsen spasticity. Incontinence occurs either as a consequence of sphincter dysfunction or from bowel spasticity and fecal urgency.
Stanley R. Pillemer, in, 2008
You May Like: Royal Canin Multifunction Urinary And Hydrolyzed Protein Feline Canned
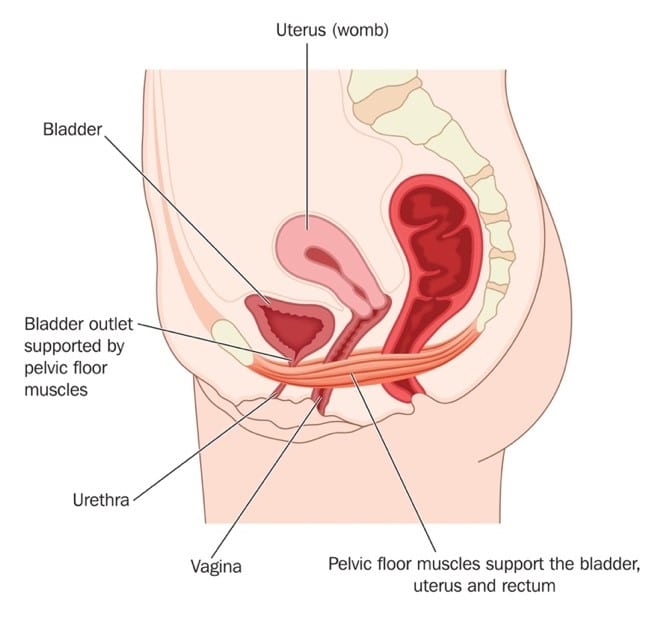
Weakened Pelvic Floor Muscles
Your pelvic floor muscles hold up many of the organs in your urinary system, including your bladder. If these muscles weaken, organs can slip slightly out of place and lead to more frequent urination. Vaginal childbirth is one way the pelvic floor muscles can become strained and start to lose their strength. Aging may also lead to pelvic floor muscles weakening.
If weakened pelvic floor muscles are causing your frequent urination, your primary care doctor or OB-GYN can work with you to understand your symptoms, make treatment recommendations and, if needed, connect you with a urogynecologist .
Read Also: Help For Female Urinary Incontinence
Read Also: Ams 800 Urinary Control System
How Is Urinary Incontinence Treated
You and your doctor or nurse will work together to create a treatment plan. You may start with steps you can take at home. If these steps do not improve your symptoms, your doctor or nurse may recommend other treatments depending on whether you have stress incontinence or urge incontinence or both.
Be patient as you work with your doctor or nurse on a treatment plan. It may take a month or longer for different treatments to begin working.
What Is Female Incontinence
Female incontinence is the loss of bladder control in women. It is not uncommon to lose urine during pregnancy or with urinary tract infections temporarily. There are many reasons you might develop urinary incontinence as a chronic problem. The most common causes are pelvic floor trauma with childbirth, menopause, hysterectomy, obesity, cognitive impairment, chronic cough and constipation.
There are three types of female incontinence:
- Urge incontinence: Women with urge incontinence feel the need to urinate frequently. They experience leakage of urine during times associated with this urge.
- Stress incontinence: Women with stress incontinence, also known as physical or exertion incontinence, may experience urine leakage, especially when coughing, laughing, exercising or sneezing.
- Mixed incontinence: Many women experience a combination of stress incontinence and urge incontinence.
Recommended Reading: Hills Science Diet Urinary Care
Duration Of Urinary Incontinence
Most cases of UI are chronic, and will remain so until treated. Depending on the cause, however, not all UI cases are chronic. If the cause is temporary, such as a vaginal infection or a urinary tract infection, the UI will stop once the issue is addressed.
RELATED: What Do the Color and Smell of Your Urine Tell You?
Diagnosing The Cause Of Frequent Urination
If urinary frequency interferes with your lifestyle or is accompanied by other symptoms such as fever, back or side pain, vomiting, chills, increased appetite or thirst, fatigue, bloody or cloudy urine, or a discharge from the or , its important to see your doctor.
To diagnose the cause of frequent urination, your doctor will perform a physical exam and take a medical history, asking questions such as the following:
- Are you taking any medications?
- Are you experiencing other symptoms?
- Do you have the problem only during the day or also at night?
- Are you drinking more than usual?
- Is your urine darker or lighter than usual?
- Do you drink alcohol or caffeinated beverages?
Depending on the findings of the physical exam and medical history, your doctor may order tests, including:
Blood Tests. Routine blood test can check for kidney function, electrolytes, and blood sugars
Urinalysis. The microscopic examination of urine that also involves a number of tests to detect and measure various compounds that pass through the urine.
Cystometry. A test that measures the pressure inside of the bladder to see how well the bladder is working cystometry is done to determine if a muscle or nerve problem may be causing problems with how well the bladder holds or releases urine. Thereâs a broader term called urodynamics that includes tests such as cystometry, uroflowmetry, urethral pressure and others.
Also Check: Urinary Tract Medication For Cats
You May Like: H Pylori Urinary Tract Infection
Finding The Right Care
Pelvic pain is a lot more common than people think, Prechel said. In Julies case, the prolonged sitting on a bike seat led to a lot of compression on her pudendal nerve. This caused pain and muscle tightness. This can also happen to men and women who spend a lot of time in the car, or who sit at a desk for work all day.
Prechel also saw patients who were experiencing pelvic pain for other reasons, including childbirth, hip or back injuries, or abdominal surgeries. She said people often live in unnecessary pain due to the sensitive nature of the injury and the treatment.
There are several physical therapists in our system who do this type of therapy for both men and women. We all respect peoples modesty, she said.Once the issue was identified, Julie and Mary began working together on a plan to relieve her pain.
Read Also: How To Cure A Urinary Tract Infection In A Woman
Other Types Of Bladder Leakage
- Mixed Incontinence: This label is given to bladder leakage conditions that stem from more than one form of incontinence, whether stress, urge, functional, or overflow. Women can be often diagnosed with stress and urge incontinence at the same time.
- Transient Incontinence: A transient incontinence refers to a temporary condition of a bladder leakage. It is often seen with complications after surgery, an irritated bladder, chronic constipation, and as a side effect of some diuretic and sleep-induced medication.
- Total Incontinence: A total loss of bladder function is referred to as total incontinence. This may be a result of nerve or bladder damage or disease that hinders the regular functioning of the bladder. Some cases of multiple sclerosis and spinal cord injuries may see a malfunction of the bladder to store urine.
You May Like: Urinary Tract Infection Not Going Away
Urinary Incontinence In Women: What You Need To Know
-
Urinary incontinence is the accidental loss of urine.
-
Over 25 million adult Americans experience temporary or chronic urinary incontinence.
-
This condition can occur at any age, but it is more common in women over the age of 50.
-
There are four types of urinary incontinence: urgency, stress, functional and overflow incontinence.
-
Behavioral therapies, medications, nerve stimulation and surgery are some of the treatments available for managing urinary incontinence.
Should I Drink Less Water Or Other Fluids If I Have Urinary Incontinence
No. Many people with urinary incontinence think they need to drink less to reduce how much urine leaks out. But you need fluids, especially water, for good health.
Women need 91 ounces of fluids a day from food and drinks.11 Getting enough fluids helps keep your kidneys and bladder healthy, prevents urinary tract infections, and prevents constipation, which may make urinary incontinence worse.
After age 60, people are less likely to get enough water, putting them at risk for dehydration and conditions that make urinary incontinence worse.12
Recommended Reading: Why Do Older Adults Get Urinary Tract Infections